Effects of propranolol treatment on left ventricular function and intracellular calcium regulation in rats with postinfarction heart failure
- PMID: 10455325
- PMCID: PMC1566147
- DOI: 10.1038/sj.bjp.0702701
Effects of propranolol treatment on left ventricular function and intracellular calcium regulation in rats with postinfarction heart failure
Abstract
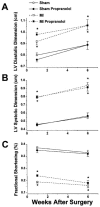
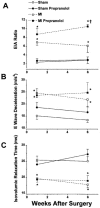
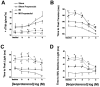
1. Chronic treatment with beta-adrenergic blocking agents can improve survival in patients with heart failure. The mechanisms underlying the beneficial effects and whether these effects are generalizable to ischaemic heart failure are unresolved. 2. We performed echocardiographic-Doppler examinations in rats (n=28) 1 and 6 weeks after myocardial infarction (MI) or sham surgery. Rats were randomized to no treatment or propranolol (500 mg/l in drinking water) after the first echocardiogram. Isometric contractions and intracellular Ca transients were recorded simultaneously in noninfarcted left ventricular (LV) papillary muscles. 3. Untreated MI rats had significant LV dilatation (10.6+/-0.4* vs 8.9+/(-0.3) mm, MI vs control), impaired systolic function (fractional shortening=11+/-2* vs 38+/-2%), and a restrictive LV diastolic filling pattern. MI rats receiving propranolol had similar LV chamber sizes (10.6+/(-0.5) mm) and systolic function (13+/(-2%). The propranolol treated animals had higher LV end-diastolic pressures (27+/-2* vs 20+/(-3 mmHg) and a more restricted LV diastolic filling pattern (increased ratio of early to late filling velocities and more rapid E wave deceleration rate). Contractility of papillary muscles from untreated MI rats was depressed (1.6+/(-0.3) vs 2.4+/(0.5 g mm(-2). In addition, Ca transients were prolonged and the inotropic response to isoproterenol was blunted. Propranolol treatment did not improve force development (1.6+/(-0.3 g mm(-2) or the duration of Ca transients during isoproterenol stimulation. 4. Chronic propranolol treatment in rats with postinfarction heart failure did not improve LV remodeling or systolic function. LV diastolic pressures and filling patterns were worsened by propranolol. Treatment also did not produce appreciable improvement in contractility, intracellular Ca regulation or beta-adrenergic responsiveness in the noninfarcted myocardium.
Figures
Similar articles
-
Clinical aspects of left ventricular diastolic function assessed by Doppler echocardiography following acute myocardial infarction.Dan Med Bull. 2001 Nov;48(4):199-210. Dan Med Bull. 2001. PMID: 11767125 Review.
-
Captopril enhances intracellular calcium handling and beta-adrenergic responsiveness of myocardium from rats with postinfarction failure.Circ Res. 1992 Oct;71(4):797-807. doi: 10.1161/01.res.71.4.797. Circ Res. 1992. PMID: 1325296
-
Long-term captopril treatment improves diastolic filling more than systolic performance in rats with large myocardial infarction.J Am Coll Cardiol. 1996 Sep;28(3):773-81. doi: 10.1016/0735-1097(96)00215-x. J Am Coll Cardiol. 1996. PMID: 8772771
-
Differential effects of mibefradil, verapamil, and amlodipine on myocardial function and intracellular Ca(2+) handling in rats with chronic myocardial infarction.J Pharmacol Exp Ther. 1999 Dec;291(3):1038-44. J Pharmacol Exp Ther. 1999. PMID: 10565822
-
Testosterone deficiency prevents left ventricular contractility dysfunction after myocardial infarction.Mol Cell Endocrinol. 2018 Jan 15;460:14-23. doi: 10.1016/j.mce.2017.06.011. Epub 2017 Jun 9. Mol Cell Endocrinol. 2018. PMID: 28606867 Review.
Cited by
-
Effects of different beta adrenoceptor ligands in mice with permanent occlusion of the left anterior descending coronary artery.Br J Pharmacol. 2003 Apr;138(8):1505-16. doi: 10.1038/sj.bjp.0705205. Br J Pharmacol. 2003. PMID: 12721106 Free PMC article.
-
Mechanisms of the beneficial effects of beta-adrenoceptor antagonists in congestive heart failure.Exp Clin Cardiol. 2010 Winter;15(4):e86-95. Exp Clin Cardiol. 2010. PMID: 21264074 Free PMC article.
-
Mineralocorticoid and AT1 receptors in the paraventricular nucleus contribute to sympathetic hyperactivity and cardiac dysfunction in rats post myocardial infarct.J Physiol. 2014 Aug 1;592(15):3273-86. doi: 10.1113/jphysiol.2014.276584. Epub 2014 Jun 20. J Physiol. 2014. PMID: 24951624 Free PMC article.
References
-
- ANDERSSON B., BLOMSTROM-LUNDQVIST C., HEDNER T., WAAGSTEIN F. Exercise hemodynamics and myocardial metabolism during long-term beta-adrenergic blockade in severe heart failure. J. Am. Coll. Cardiol. 1991;18:1059–1066. - PubMed
-
- APPLETON C., HATLE L., POPP R. Relation of transmitral flow velocity patterns to left ventricular diastolic function: new insights from a combined hemodynamic and echocardiographic study. J. Am. Coll. Cardiol. 1988;12:426–440. - PubMed
-
- AUSTRALIA/NEWZEALAND HEART FAILURE RESEARCH COLLABORATIVE GROUP Randomized, placebo-controlled trial of carvedilol in patients with congestive heart failure due to ischaemic heart disease. Lancet. 1997;349:375–380. - PubMed
-
- BART B.A., SHAW L.K., MCCANTS C.B., FORTIN D.F., LEE K.L., CALIFF R.M., O'CONNOR C.M. Clinical determinants of mortality in patients with angiographically diagnosed ischemic or nonischemic cardiomyopathy. J. Am. Coll. Cardiol. 1997;30:1002–1008. - PubMed
-
- BETA BLOCKER HEART ATTACK TRIAL RESEARCH GROUP A randomized trial of propranolol in patients with acute myocardial infarction. JAMA. 1982;247:1707–1713. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

