Inadequate ischaemia-selectivity limits the antiarrhythmic efficacy of mibefradil during regional ischaemia and reperfusion in the rat isolated perfused heart
- PMID: 10498833
- PMCID: PMC1571614
- DOI: 10.1038/sj.bjp.0702778
Inadequate ischaemia-selectivity limits the antiarrhythmic efficacy of mibefradil during regional ischaemia and reperfusion in the rat isolated perfused heart
Abstract
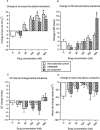
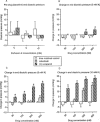
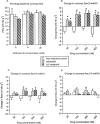
1. Mibefradil was compared with (+/-)-verapamil for effects on ischaemia- and reperfusion-induced ventricular fibrillation (VF), and the role of ischaemia-selective L-channel block was examined. Langendorff perfused rat hearts (n=12/group) were used. 2. Neither drug at up to 100 nM reduced the incidence of VF during 30 min regional ischaemia. 300 and 600 nM (+/-)-verapamil abolished VF (P<0. 05); mibefradil was effective only at 600 nM (P<0.05). Reperfusion-induced VF incidence was reduced only by 600 nM (+/-)-verapamil (P<0.05). Both drugs at >/=100 nM increased coronary flow (P<0.05) with a similar potency and maximum effectiveness. 3. In separate hearts perfused with Krebs' solution containing 3 mM K+ (the same as that used for arrhythmia studies) neither drug at up to 600 nM affected ventricular contractility. With K+ raised to 6 mM, (+/-)-verapamil >/=30 nM reduced developed pressure (P<0.05); mibefradil did so only at 600 nM (P<0.05). With K+ raised to 10 mM the effects of (+/-)-verapamil were further increased (P<0.05) and mibefradil became active at >/=100 nM (P<0.05). Likewise both drugs impaired diastolic relaxation, with raised K+ exacerbating the effects and (+/-)-verapamil being more potent and its effects more greatly exacerbated by K+. In contrast, when K+ was normal (3 mM), coronary flow was increased by each drug at >/=30 nM (P<0.05) indicating a marked vascular : myocardial selectivity. 4. In conclusion, mibefradil differed from (+/-)-verapamil in its myocardial effects only in terms of its lower potency. As mibefradil is the more potent T-channel blocker, the T-channel is unlikely to represent the molecular target for these effects. The K+ elevations that occur in the ischaemic milieu determine the ability of both drugs to block myocardial L-channels; this is sufficient to account for the drugs' actions on VF. Neither drug possesses sufficient selectivity for ischaemic myocardium versus blood vessels to permit efficacy (VF suppression without marked vasodilatation) and so inappropriate hypotension is likely to preclude the safe use of mibefradil (or similar analogue) in VF suppression, and explains the lack of clinical effectiveness of (+/-)-verapamil.
Figures

Similar articles
-
Mibefradil is more effective than verapamil for restoring post-ischemic function of isolated hearts of guinea pigs with acute renal failure.Eur J Pharmacol. 2004 Mar 19;488(1-3):137-46. doi: 10.1016/j.ejphar.2004.02.013. Eur J Pharmacol. 2004. PMID: 15044045
-
Comparison of effects of nitrendipine, lacidipine and mibefradil on postischaemic myocardial damage in isolated rat hearts.Pflugers Arch. 2000;440(5 Suppl):R149-50. Pflugers Arch. 2000. PMID: 11005649
-
Effects of mibefradil, a novel calcium channel blocking agent with T-type activity, in acute experimental myocardial ischemia: maintenance of ventricular fibrillation threshold without inotropic compromise.J Am Coll Cardiol. 1998 Jul;32(1):268-74. doi: 10.1016/s0735-1097(98)00182-x. J Am Coll Cardiol. 1998. PMID: 9669280
-
Comparative pharmacological properties among calcium channel blockers: T-channel versus L-channel blockade.Cardiology. 1998;89 Suppl 1:10-5. doi: 10.1159/000047274. Cardiology. 1998. PMID: 9570424 Review.
-
Myocardial protection with calcium-channel blockers during ischaemia and reperfusion by PTCA.Eur Heart J. 1995 Aug;16 Suppl H:3-8. doi: 10.1093/eurheartj/16.suppl_h.3. Eur Heart J. 1995. PMID: 8846802 Review.
Cited by
-
Contractile function assessment by intraventricular balloon alters the ability of regional ischaemia to evoke ventricular fibrillation.Br J Pharmacol. 2016 Jan;173(1):39-52. doi: 10.1111/bph.13332. Epub 2015 Dec 4. Br J Pharmacol. 2016. PMID: 26377788 Free PMC article.
-
Na(+)/Ca(2+) exchanger inhibition exerts a positive inotropic effect in the rat heart, but fails to influence the contractility of the rabbit heart.Br J Pharmacol. 2008 May;154(1):93-104. doi: 10.1038/bjp.2008.83. Epub 2008 Mar 10. Br J Pharmacol. 2008. PMID: 18332852 Free PMC article.
-
Feasibility of targeting ischaemia-related ventricular arrhythmias by mimicry of endogenous protection by endocannabinoids.Br J Pharmacol. 2013 Aug;169(8):1840-8. doi: 10.1111/bph.12252. Br J Pharmacol. 2013. PMID: 23713981 Free PMC article.
-
Absolute beat-to-beat variability and instability parameters of ECG intervals: biomarkers for predicting ischaemia-induced ventricular fibrillation.Br J Pharmacol. 2014 Apr;171(7):1772-82. doi: 10.1111/bph.12579. Br J Pharmacol. 2014. PMID: 24417376 Free PMC article.
-
Nupafant, a PAF-antagonist prototype for suppression of ventricular fibrillation without liability for QT prolongation?Br J Pharmacol. 2006 Oct;149(3):269-76. doi: 10.1038/sj.bjp.0706846. Epub 2006 Aug 21. Br J Pharmacol. 2006. PMID: 16921398 Free PMC article.
References
-
- ANTMAN E.M., LAU J., KUPELNICK B., MOSTELLER F., CHALMERS T.C. A comparison of results of meta analyses of randomized control trials and recommendations of clinical experts: treatments for myocardial infarction. J. Am. Med. Assoc. 1992;268:240–248. - PubMed
-
- BEZPROZVANNY L., TSIEN R.W. Voltage-dependent blockade of diverse types of voltage-gated Ca2+ channels expressed in Ixenopus oocytes by the Ca2+ channel antagonist mibefradil (Ro-40-5967) Mol. Pharmacol. 1995;48:540–549. - PubMed
-
- BILLMAN G.E. The effect of Ro-40 5967, a novel calcium channel antagonist on susceptibility to ventricular fibrillation. Circulation. 1991;84 Suppl. II:2183.
-
- BILLMAN G.E., HAMLIN R.L. The effects of mibefradil, a novel calcium channel antagonist on ventricular arrhythmias induced by myocardial ischemia and programmed electrical stimulation. J. Pharm. Exp. Ther. 1996;277:1517–1526. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

