Cyclin-dependent kinases as a therapeutic target for stroke
- PMID: 10944192
- PMCID: PMC27851
- DOI: 10.1073/pnas.170144197
Cyclin-dependent kinases as a therapeutic target for stroke
Abstract
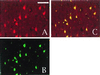
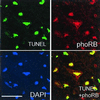
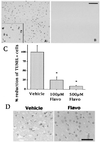
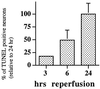
Cyclin-dependent kinases (CDKs) are commonly known to regulate cell proliferation. However, previous reports suggest that in cultured postmitotic neurons, activation of CDKs is a signal for death rather than cell division. We determined whether CDK activation occurs in mature adult neurons during focal stroke in vivo and whether this signal was required for neuronal death after reperfusion injury. Cdk4/cyclin D1 levels and phosphorylation of its substrate retinoblastoma protein (pRb) increase after stroke. Deregulated levels of E2F1, a transcription factor regulated by pRb, are also observed. Administration of a CDK inhibitor blocks pRb phosphorylation and the increase in E2F1 levels and dramatically reduces neuronal death by 80%. These results indicate that CDKs are an important therapeutic target for the treatment of reperfusion injury after ischemia.
Figures



Similar articles
-
Involvement of retinoblastoma family members and E2F/DP complexes in the death of neurons evoked by DNA damage.J Neurosci. 2000 May 1;20(9):3104-14. doi: 10.1523/JNEUROSCI.20-09-03104.2000. J Neurosci. 2000. PMID: 10777774 Free PMC article.
-
Direct interaction of p21 cyclin-dependent kinase inhibitor with the retinoblastoma tumor suppressor protein.Biochem Biophys Res Commun. 1999 Sep 16;263(1):35-40. doi: 10.1006/bbrc.1999.1296. Biochem Biophys Res Commun. 1999. PMID: 10486249
-
Involvement of cell cycle elements, cyclin-dependent kinases, pRb, and E2F x DP, in B-amyloid-induced neuronal death.J Biol Chem. 1999 Jul 2;274(27):19011-6. doi: 10.1074/jbc.274.27.19011. J Biol Chem. 1999. PMID: 10383401
-
[Molecular mechanisms controlling the cell cycle: fundamental aspects and implications for oncology].Cancer Radiother. 2001 Apr;5(2):109-29. doi: 10.1016/s1278-3218(01)00087-7. Cancer Radiother. 2001. PMID: 11355576 Review. French.
-
Melanoma cell autonomous growth: the Rb/E2F pathway.Cancer Metastasis Rev. 1999;18(3):333-43. doi: 10.1023/a:1006396104073. Cancer Metastasis Rev. 1999. PMID: 10721488 Review.
Cited by
-
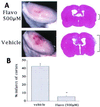
Neuroprotective and anti-inflammatory effects of the flavonoid-enriched fraction AF4 in a mouse model of hypoxic-ischemic brain injury.PLoS One. 2012;7(12):e51324. doi: 10.1371/journal.pone.0051324. Epub 2012 Dec 12. PLoS One. 2012. PMID: 23251498 Free PMC article.
-
Remote Ischemic Conditioning Alters Methylation and Expression of Cell Cycle Genes in Aneurysmal Subarachnoid Hemorrhage.Stroke. 2015 Sep;46(9):2445-51. doi: 10.1161/STROKEAHA.115.009618. Epub 2015 Aug 6. Stroke. 2015. PMID: 26251247 Free PMC article. Clinical Trial.
-
Inhibition of the JAK2/STAT3 pathway and cell cycle re-entry contribute to the protective effect of remote ischemic pre-conditioning of rat hindlimbs on cerebral ischemia/reperfusion injury.CNS Neurosci Ther. 2023 Mar;29(3):866-877. doi: 10.1111/cns.14023. Epub 2022 Nov 23. CNS Neurosci Ther. 2023. PMID: 36419252 Free PMC article.
-
Identification of Sleep-Modulated Pathways Involved in Neuroprotection from Stroke.Sleep. 2015 Nov 1;38(11):1707-18. doi: 10.5665/sleep.5148. Sleep. 2015. PMID: 26085290 Free PMC article.
-
Alterations in cyclin A, B, and D1 in mouse dentate gyrus following TMT-induced hippocampal damage.Neurotox Res. 2003;5(5):339-54. doi: 10.1007/BF03033154. Neurotox Res. 2003. PMID: 14715453
References
-
- Choi D W. Neuron. 1988;1:623–634. - PubMed
-
- Dirnagl U, Iadecola C, Moskowitz M A. Trends Neurosci. 1999;22:391–397. - PubMed
-
- MacManus J P, Hill I E, Preston E, Rasquinha I, Walker T, Buchan A M. J Cereb Blood Flow Metab. 1995;15:728–737. - PubMed
-
- Lipton P. Physiol Rev. 1999;79:1431–1568. - PubMed
-
- Pines J. Biochem Soc Trans. 1993;21:921–925. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

