Trehalose 6,6'-dimycolate (cord factor) of Mycobacterium tuberculosis induces corneal angiogenesis in rats
- PMID: 10992511
- PMCID: PMC101563
- DOI: 10.1128/IAI.68.10.5991-5997.2000
Trehalose 6,6'-dimycolate (cord factor) of Mycobacterium tuberculosis induces corneal angiogenesis in rats
Abstract
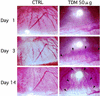
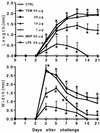
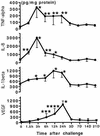
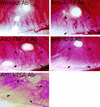
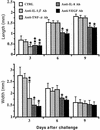
Neovascularization or angiogenesis is required for the progression of chronic inflammation. The mechanism of inflammatory neovascularization in tuberculosis remains unknown. Trehalose 6, 6'-dimycolate (TDM) purified from Mycobacterium tuberculosis was injected into rat corneas. TDM challenge provoked a local granulomatous response in association with neovascularization. Neovascularization was seen within a few days after the challenge, with the extent of neovascularization being dose dependent, although granulomatous lesions developed 14 days after the challenge. Cytokines, including tumor necrosis factor alpha (TNF-alpha), interleukin-8 (IL-8), IL-1beta, and vascular endothelial growth factor (VEGF), were found in lesions at the early stage (within a few days after the challenge) and were detectable until day 21. Neovascularization was inhibited substantially by neutralizing antibodies to VEGF and IL-8 but not IL-1beta. Treatment with anti-TNF-alpha antibodies resulted in partial inhibition. TDM possesses pleiotropic activities, and the cytokine network plays an important role in the process of neovascularization.
Figures

Similar articles
-
A role for tumour necrosis factor-alpha, complement C5 and interleukin-6 in the initiation and development of the mycobacterial cord factor trehalose 6,6'-dimycolate induced granulomatous response.Microbiology (Reading). 2008 Jun;154(Pt 6):1813-1824. doi: 10.1099/mic.0.2008/016923-0. Microbiology (Reading). 2008. PMID: 18524936 Free PMC article.
-
Trehalose 6,6'-dimycolate (Cord factor) enhances neovascularization through vascular endothelial growth factor production by neutrophils and macrophages.Infect Immun. 2000 Apr;68(4):2043-52. doi: 10.1128/IAI.68.4.2043-2052.2000. Infect Immun. 2000. PMID: 10722600 Free PMC article.
-
Cytokine message and protein expression during lung granuloma formation and resolution induced by the mycobacterial cord factor trehalose-6,6'-dimycolate.J Interferon Cytokine Res. 2000 Sep;20(9):795-804. doi: 10.1089/10799900050151067. J Interferon Cytokine Res. 2000. PMID: 11032399
-
Immunological properties of trehalose dimycolate (cord factor) and other mycolic acid-containing glycolipids--a review.Microbiol Immunol. 2001;45(12):801-11. doi: 10.1111/j.1348-0421.2001.tb01319.x. Microbiol Immunol. 2001. PMID: 11838897 Review.
-
[Up-to-date understanding of tuberculosis immunity].Kekkaku. 2003 Jan;78(1):51-5. Kekkaku. 2003. PMID: 12683337 Review. Japanese.
Cited by
-
Macrophage NFATC2 mediates angiogenic signaling during mycobacterial infection.Cell Rep. 2022 Dec 13;41(11):111817. doi: 10.1016/j.celrep.2022.111817. Cell Rep. 2022. PMID: 36516756 Free PMC article.
-
Cyclopropane Modification of Trehalose Dimycolate Drives Granuloma Angiogenesis and Mycobacterial Growth through Vegf Signaling.Cell Host Microbe. 2018 Oct 10;24(4):514-525.e6. doi: 10.1016/j.chom.2018.09.004. Cell Host Microbe. 2018. PMID: 30308157 Free PMC article.
-
Adventures within the speckled band: heterogeneity, angiogenesis, and balanced inflammation in the tuberculous granuloma.Immunol Rev. 2015 Mar;264(1):276-87. doi: 10.1111/imr.12273. Immunol Rev. 2015. PMID: 25703566 Free PMC article. Review.
-
Interferon-gamma independent formation of pulmonary granuloma in mice by injections with trehalose dimycolate (cord factor), lipoarabinomannan and phosphatidylinositol mannosides isolated from Mycobacterium tuberculosis.Clin Exp Immunol. 2006 Apr;144(1):134-41. doi: 10.1111/j.1365-2249.2006.03043.x. Clin Exp Immunol. 2006. PMID: 16542375 Free PMC article.
-
Effects of endostatin-vascular endothelial growth inhibitor chimeric recombinant adenoviruses on antiangiogenesis.World J Gastroenterol. 2004 May 15;10(10):1409-14. doi: 10.3748/wjg.v10.i10.1409. World J Gastroenterol. 2004. PMID: 15133844 Free PMC article.
References
-
- Amano S, Rohan R, Kuroki M, Tolentino M, Adamis A P. Requirement for vascular endothelial growth factor in wound- and inflammation-related corneal neovascularization. Investig Ophthalmol Vis Sci. 1998;39:18–22. - PubMed
-
- Baggiolini M, Dewald B, Moser B. Human chemokines: an update. Annu Rev Immunol. 1997;15:675–705. - PubMed
-
- Besra G S, Chatterjee D. Lipids and carbohydrates of Mycobacterium tuberculosis. In: Bloom B R, editor. Tuberculosis: pathogenesis, protection, and control. Washington, D.C.: ASM Press; 1994. pp. 285–306.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

