Uteroplacental blood flow. The story of decidualization, menstruation, and trophoblast invasion
- PMID: 11106547
- PMCID: PMC1885765
- DOI: 10.1016/S0002-9440(10)64813-4
Uteroplacental blood flow. The story of decidualization, menstruation, and trophoblast invasion
Figures
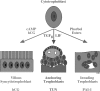


References
-
- Benirschke K, Kaufmann P: Pathology of the Human Placenta, 3d edition. 1995. Springer-Verlag, New York
-
- Thornburg KL, Jacobson SL, Giraud GD, Morton MJ: Hemodynamic changes in pregnancy. Semin Perinatol 2000, 24:11-14 - PubMed
-
- Duvekot JJ, Peeters LL: Maternal cardiovascular hemodynamic adaptation to pregnancy. Obstet Gynecol Surv 1994, 49:S1-S14 - PubMed
-
- Naeye RL: Pregnancy hypertension, placental evidences of low uteroplacental blood flow, and spontaneous premature delivery. Hum Pathol 1989, 20:441-444 - PubMed
-
- Silver M, Barnes RJ, Comline RS, Burton GJ: Placental blood flow: some fetal and maternal cardiovascular adjustments during gestation. J Reprod Fertil Suppl 1982, 31:139-160 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

