MR imaging of the cauda equina in hereditary motor sensory neuropathies: correlations with sural nerve biopsy
- PMID: 11110529
- PMCID: PMC7974297
MR imaging of the cauda equina in hereditary motor sensory neuropathies: correlations with sural nerve biopsy
Abstract
Background and purpose: Although spinal root abnormalities are known to occur, spinal MR examination is seldom performed in hereditary motor and sensory neuropathies (HMSN). The following work was undertaken to assess the MR imaging spectrum of lumbosacral spinal nerve root abnormalities and determine whether intradural nerve root involvement could be related to any biopsy feature.
Methods: Ten consecutive patients (eight male, two female; age range, 28-65 yrs) with Charcot-Marie-Tooth (CMT) (type I = 5, type II = 2) and Déjèrine-Sottas disease (DSD) (n = 3) underwent a contrast-enhanced lumbosacral MR examination. Sural nerve biopsy was performed in all patients. Atypical clinical features were present in two patients. The MR scans of each patient were reviewed for possible causes of myeloradiculopathy, spinal nerve root and ganglia dimensions, signal change, and abnormal enhancement.
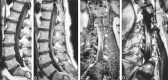
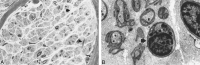
Results: In the seven patients with CMT, abnormal MR findings were intradural nerve root hypertrophy (n = 2), signal abnormalities (n = 2), and enhancement (n = 3). Two of three patients with DSD had the abnormal MR finding of intradural nerve root enhancement. In both patients with atypical clinical features, MR imaging showed nerve root hypertrophy and enhancement. Both findings were related to an increased number of onion bulbs at sural nerve biopsy. Inflammatory infiltrates were not observed in any patients.
Conclusion: In patients with HMSN enhancement of intradural spinal nerve roots, whether or not associated with marked thickening, may be found on lumbosacral MR examinations. Spinal nerve root thickening may be responsible for atypical symptoms, and its visibility on MR images represents a useful adjunct to diagnosis. Lumbosacral spinal nerve root abnormalities were related to an extremely high number of onion bulbs (indicating active demyelination) at sural nerve biopsy. Nerve root enhancement does not seem to be related to inflammatory infiltrates.
Figures


Comment in
-
Is there room for MR imaging in the assessment of hereditary motor and sensory neuropathies?AJNR Am J Neuroradiol. 2000 Nov-Dec;21(10):1779-80. AJNR Am J Neuroradiol. 2000. PMID: 11110525 Free PMC article. No abstract available.
Similar articles
-
MR imaging of Dejerine-Sottas disease.AJNR Am J Neuroradiol. 1999 Mar;20(3):378-80. AJNR Am J Neuroradiol. 1999. PMID: 10219400 Free PMC article.
-
Hypertrophic motor and sensory neuropathy type I (Charcot-Marie-Tooth disease): ultrastructural study of sural nerve biopsy in members of a family.Pathologica. 1994 Jun;86(3):279-83. Pathologica. 1994. PMID: 7808799
-
Is there room for MR imaging in the assessment of hereditary motor and sensory neuropathies?AJNR Am J Neuroradiol. 2000 Nov-Dec;21(10):1779-80. AJNR Am J Neuroradiol. 2000. PMID: 11110525 Free PMC article. No abstract available.
-
Four novel cases of periaxin-related neuropathy and review of the literature.Neurology. 2010 Nov 16;75(20):1830-8. doi: 10.1212/WNL.0b013e3181fd6314. Neurology. 2010. PMID: 21079185 Review.
-
Hypertrophied cauda equina presenting as intradural mass: case report and review of literature.Surg Neurol. 1998 May;49(5):514-8; discussion 518-9. doi: 10.1016/s0090-3019(97)00160-2. Surg Neurol. 1998. PMID: 9586929 Review.
Cited by
-
Sibling Cases of Charcot-Marie-Tooth Disease Type 4H with a Homozygous FGD4 Mutation and Cauda Equina Thickening.Intern Med. 2021 Dec 15;60(24):3975-3981. doi: 10.2169/internalmedicine.7247-21. Epub 2021 Jun 19. Intern Med. 2021. PMID: 34148957 Free PMC article.
-
Acute to Subacute Atraumatic Entrapment Neuropathies in Patients With CMT1A: A Report of a Distinct Phenotypic Variant of CMT1A.Front Neurol. 2022 Feb 25;13:826634. doi: 10.3389/fneur.2022.826634. eCollection 2022. Front Neurol. 2022. PMID: 35280294 Free PMC article.
-
Autoimmune neuromuscular disorders in childhood.Curr Treat Options Neurol. 2011 Dec;13(6):590-607. doi: 10.1007/s11940-011-0146-5. Curr Treat Options Neurol. 2011. PMID: 21912840 Free PMC article.
-
Autosomal Recessive Spastic Ataxia of Charlevoix-Saguenay due to Novel Mutations in the SACS Gene.J Investig Med High Impact Case Rep. 2022 Jan-Dec;10:23247096221139670. doi: 10.1177/23247096221139670. J Investig Med High Impact Case Rep. 2022. PMID: 36458808 Free PMC article.
-
Ultrasonographic nerve enlargement of the median and ulnar nerves and the cervical nerve roots in patients with demyelinating Charcot-Marie-Tooth disease: distinction from patients with chronic inflammatory demyelinating polyneuropathy.J Neurol. 2013 Oct;260(10):2580-7. doi: 10.1007/s00415-013-7021-0. Epub 2013 Jul 3. J Neurol. 2013. PMID: 23821028
References
-
- Masuda N, Hayashi H, Tanabe H. Nerve root and sciatic trunk enlargement in Dejerine-Sottas disease: MRI appearance. Neuroradiology 1992;35:36-37 - PubMed
-
- Murata K, Morishita S, Nakamuro T, Kanda T, Takayanagi T. A case report of the compression syndrome due to hypertrophic neuropathy. Clin Neurol 1991;31:213-215 - PubMed
-
- Tachi N, Kozuka N, Ohya K, Chiba S, Naganuma M. MRI of peripheral nerves and pathology of sural nerves in hereditary motor and sensory neuropathy type III. Neuroradiology 1995;37:496-499 - PubMed
-
- Friedman DP, Flanders AE, Tartaglino LM. Hypertrophic Charcot-Marie-Tooth disease: MR imaging findings. AJR Am J Roentgenol 1994;163:749-750 - PubMed
-
- Rosen SA, Wang H, Cornblath DR, Uematsu E, Hurko O. Compression syndromes due to hypertrophic nerve roots in hereditary motor sensory neuropathy type I. Neurology 1989;39:1173-1177 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
