Left ventricular stroke volume in the fetal sheep is limited by extracardiac constraint and arterial pressure
- PMID: 11507172
- PMCID: PMC2278767
- DOI: 10.1111/j.1469-7793.2001.t01-1-00231.x
Left ventricular stroke volume in the fetal sheep is limited by extracardiac constraint and arterial pressure
Abstract
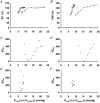
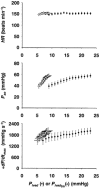
1. Extracardiac constraint and sensitivity to arterial pressure may be critical factors that limit the functional reserves of the developing fetal heart in utero. We hypothesise that extracardiac constraint is the predominant factor that limits fetal stroke volume (SV). To test this hypothesis we studied six chronically instrumented fetal sheep to determine the relative roles that extracardiac constraint and arterial pressure play in determining left ventricular (LV) function. 2. Pregnant ewes (128-131 days gestation, term = 147 days) were anaesthetised (5 mg kg(-1) Propofol I.V., then 1.5 % halothane, 50 % O(2), balance N(2)O by inhalation) and instrumented using sterile surgical techniques to record LV end-diastolic pressure (P(lved)), aortic pressure (P(ao)), pericardial pressure (P(per)), and LV SV. 3. After a minimum of 72 h recovery, LV function was assessed by altering fetal blood volume to vary P(lved). Ventricular function curves were generated using two measures of ventricular function, SV and stroke work index (SWI = SV x P(ao)), and two measures of ventricular filling, P(lved) and LV end-diastolic transmural pressure (P(lved,tm) = P(lved) - P(per)). 4. Although decreasing P(lved) from the resting level decreased SV, increasing P(lved) from the resting level did not increase SV because the ventricular function curve plateaued. This plateau was not explained solely by an increase in aortic pressure, as the plateau remained present in the SWI versus P(lved) curve. When extracardiac constraint was accounted for (SV against P(lved,tm)), the plateau was largely eliminated (approximately 80 %). The remaining portion of the plateau (approximately 20 %) was eliminated when both extracardiac constraint and arterial pressure were accounted for (SWI versus P(lved,tm)). 5. Thus, the major limitation upon LV function in the near-term fetus results from extracardiac constraint limiting ventricular filling while, at the same time, a much smaller limitation arises from increasing arterial pressure.
Figures

References
-
- Anderson P A W, Manring A, Glick K L, Crenshaw C C. Biophysics of the developing heart. III. A comparison of the left ventricular dynamics of the fetal and neonatal lamb heart. American Journal of Obstetrics and Gynecology. 1982;143:195–203. - PubMed
-
- Cohn H E, Sacks E J, Heymann M A, Rudolph A M. Cardiovascular responses to hypoxemia and academia in fetal lambs. American Journal of Obstetrics and Gynecology. 1974;120:817–824. - PubMed
-
- Gilbert R D. Control of fetal cardiac output during changes in blood volume. American Journal of Physiology. 1980;238:H80–86. - PubMed
-
- Gilbert R D. Effects of afterload and baroreceptors on cardiac function in fetal sheep. Journal of Developmental Physiology. 1982;4:299–309. - PubMed
-
- Glantz S A, Parmley W W. Factors which affect the diastolic pressure-volume curve. Circulation Research. 1978;42:171–180. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

