Diagnostic and treatment characteristics of polycystic ovary syndrome: descriptive measurements of patient perception and awareness from 657 confidential self-reports
- PMID: 11545683
- PMCID: PMC55341
- DOI: 10.1186/1472-6874-1-3
Diagnostic and treatment characteristics of polycystic ovary syndrome: descriptive measurements of patient perception and awareness from 657 confidential self-reports
Abstract
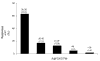
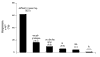
BACKGROUND: This investigation was undertaken to describe patient perception and awareness of the polycystic ovary syndrome (PCOS), the most common cause of anovulation/oligoovulation among women of reproductive age. METHODS: Fifteen parameters were evaluated by a computer-based research instrument accessed by a large, unscreened population. Incomplete questionnaires were not entered, and responses were electronically tabulated to block duplicate submissions. RESULTS: From 657 participants, the majority (63%) were between 26-34 years old; mean BMI was 30.4 kg/m2. 343 of 657 had at least one pregnancy and 61% of the study group had taken fertility medicine (any type) at least once. Physicians were the most common provider of PCOS information for all study participants, irrespective of age. Patient emotions associated with the diagnosis of PCOS included "frustration" (67%), "anxiety" (16%), "sadness" (10%), and "indifference" (2%). Self-reported patient aptitude regarding PCOS was scored as high or "very aware" in >60% of women. Respondents were also asked: "If your PCOS could be safely and effectively helped by something else besides fertility drugs or birth control pills, would that interest you?" Interest in alternative PCOS treatments was expressed by 99% of the sample (n = 648). CONCLUSIONS: In our study population, most women associated negative emotions with PCOS although the self-reported knowledge level for the disorder was high. While these women regarded their obstetrician-gynecologist as integral to their PCOS education, traditional PCOS therapies based on oral contraceptives or ovulation induction agents were regarded as unsatisfactory by most women.
Figures
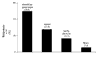




References
-
- Cronin L, Guyatt G, Griffith L, et al. Development of a health related quality of life questionnaire for women with polycystic ovary syndrome (PCOS). J Clin Endocrinol Metab. 1998;83:1976–87. - PubMed
-
- Kidson W. Polycystic ovary syndrome: a new direction in treatment. Med J Aust. 1999;169:537–40. - PubMed
-
- Jakubowicz DJ, Seppala M, Jakubowicz S, et al. Insulin reduction with metformin increases luteal phase glycodelin and insulin-like growth factor-binding protein 1 concentrations and enhances uterine vascularity and blood flow in the polycystic ovary syndrome. J Clin Endocrinol Metab. 2001;86:1126–33. - PubMed
-
- Sills ES, Levy DP, Wittkowski KM, Perloe M. Preliminary experience with metformin treatment of polycystic ovary syndrome: reproductive outcomes among 20 consecutive patients. Fertil Steril. 1999;72(Suppl 1):S187–8.
-
- Sills ES, Perloe M, Palermo GD. Correction of hyperinsulinemia in oligoovulatory women with clomiphene-resistant polycystic ovary syndrome: a review of therapeutic rationale and reproductive outcomes. Eur J Obstet Gynecol Reprod Biol. 2000;91:135–41. doi: 10.1016/S0301-2115(99)00287-0. - DOI - PubMed
LinkOut - more resources
Full Text Sources

