Therapeutic application of caspase 1/interleukin-1beta-converting enzyme inhibitor decreases the death rate in severe acute experimental pancreatitis
- PMID: 11753044
- PMCID: PMC1422397
- DOI: 10.1097/00000658-200201000-00009
Therapeutic application of caspase 1/interleukin-1beta-converting enzyme inhibitor decreases the death rate in severe acute experimental pancreatitis
Abstract
Objective: To assess the effect of therapeutic inhibition of interleukin 1beta-converting enzyme (ICE) in an experimental model of severe acute pancreatitis (SAP).
Summary background data: Several lines of evidence suggest that cytokines activated by ICE play an instrumental role in the course of acute pancreatitis. Recent studies have shown that pharmacologic or genetic blockade of ICE significantly ameliorates the overall severity of and the death rate in SAP.
Methods: Severe acute pancreatitis was induced by infusion of 5% sodium taurocholate in Wistar rats. A new, highly selective, irreversible inhibitor of ICE was intraperitoneally applied at a dosage of 0.25 mg every 12 hours. Control animals in group 1 received treatment with saline; in group 2 rats, ICE inhibition was started 6 hours after the onset of pancreatitis; and in group 3 rats, ICE inhibition was started 12 hours after the onset of pancreatitis. After a 7-day observation period, surviving rats were killed and blood, plasma, pancreas, lung, and liver were used for subsequent analysis.
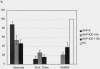
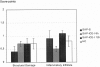
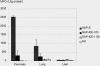
Results: Inhibition of ICE decreased the 7-day death rate from 87.5% to 38.9% irrespective whether treatment was started 6 hours or 12 hours after induction of SAP. Morphometric analysis revealed a significant reduction of acinar cell necrosis in both treated groups, whereas pancreatitis-associated pulmonary and hepatic damage was uniformly low and not influenced by ICE inhibition. Tissue myeloperoxidase concentrations were dramatically decreased in the pancreas and the lung after either regimen of ICE inhibitor treatment. In contrast to lung and liver, marked upregulation of interleukin 1beta, tumor necrosis factor alpha, and ICE mRNA was observed in the pancreas, with levels of interleukin 1beta and tumor necrosis factor alpha being reduced in ICE-inhibited animals. Compared with nontreated rats, plasma amylase levels were higher in both treatment groups, whereas lipase and hematocrit showed no difference. Changes of the differential white blood count including neutrophils, lymphocytes, and monocytes were attenuated in both groups after ICE inhibitor treatment.
Conclusions: Pharmacologic inhibition of ICE significantly improves the overall severity of and the death rate in SAP. A substantial reduction of neutrophil-mediated tissue injury in pancreas and lung seems to contribute to the beneficial effects of this approach. Moreover, ICE inhibition is still effective after a therapeutic window of 12 hours. Based on the current findings, future studies on the clinical application of ICE-inhibiting substances in acute pancreatitis seem to be promising.
Figures

Similar articles
-
Caspase-1 inhibition alleviates acute renal injury in rats with severe acute pancreatitis.World J Gastroenterol. 2014 Aug 14;20(30):10457-63. doi: 10.3748/wjg.v20.i30.10457. World J Gastroenterol. 2014. PMID: 25132762 Free PMC article.
-
Therapeutic effects of caspase-1 inhibitors on acute lung injury in experimental severe acute pancreatitis.World J Gastroenterol. 2007 Jan 28;13(4):623-7. doi: 10.3748/wjg.v13.i4.623. World J Gastroenterol. 2007. PMID: 17278232 Free PMC article.
-
Differential effects of caspase-1/interleukin-1beta-converting enzyme on acinar cell necrosis and apoptosis in severe acute experimental pancreatitis.Lab Invest. 2001 Jul;81(7):1001-13. doi: 10.1038/labinvest.3780312. Lab Invest. 2001. PMID: 11454989
-
Interleukin-18: a pro-inflammatory cytokine that plays an important role in acute pancreatitis.Expert Opin Ther Targets. 2007 Oct;11(10):1261-71. doi: 10.1517/14728222.11.10.1261. Expert Opin Ther Targets. 2007. PMID: 17907957 Review.
-
Interleukin-1beta converting enzyme (caspase-1) in intestinal inflammation.Biochem Pharmacol. 2002 Jul 1;64(1):1-8. doi: 10.1016/s0006-2952(02)01064-x. Biochem Pharmacol. 2002. PMID: 12106600 Review.
Cited by
-
Caspase-1 is hepatoprotective during trauma and hemorrhagic shock by reducing liver injury and inflammation.Mol Med. 2011 Sep-Oct;17(9-10):1031-8. doi: 10.2119/molmed.2011.00015. Epub 2011 Jun 7. Mol Med. 2011. PMID: 21666957 Free PMC article.
-
Necro-inflammatory response of pancreatic acinar cells in the pathogenesis of acute alcoholic pancreatitis.Cell Death Dis. 2013 Oct 3;4(10):e816. doi: 10.1038/cddis.2013.354. Cell Death Dis. 2013. PMID: 24091659 Free PMC article.
-
Immunomodulatory therapies for acute pancreatitis.World J Gastroenterol. 2014 Dec 7;20(45):16935-47. doi: 10.3748/wjg.v20.i45.16935. World J Gastroenterol. 2014. PMID: 25493006 Free PMC article. Review.
-
Caspase-1 inhibition alleviates acute renal injury in rats with severe acute pancreatitis.World J Gastroenterol. 2014 Aug 14;20(30):10457-63. doi: 10.3748/wjg.v20.i30.10457. World J Gastroenterol. 2014. PMID: 25132762 Free PMC article.
-
Zerumbone attenuates the severity of acute necrotizing pancreatitis and pancreatitis-induced hepatic injury.Mediators Inflamm. 2012;2012:156507. doi: 10.1155/2012/156507. Epub 2012 Mar 5. Mediators Inflamm. 2012. PMID: 22529518 Free PMC article.
References
-
- Beger HG, Rau B, Mayer J, et al. Natural course of acute pancreatitis. World J Surg 1997; 21: 130–135. - PubMed
-
- Dervenis C, Johnson CD, Bassi C, et al. Diagnosis, objective assessment of severity, and management of acute pancreatitis: Santorini consensus conference. Int J Pancreatol 1999; 25: 195–210. - PubMed
-
- Norman J. The role of cytokines in the pathogenesis of acute pancreatitis. Am J Surg 1998; 175: 76–83. - PubMed
-
- Ogawa M. Acute pancreatitis and cytokines: “Second attack” by septic complications leads to organ failure. Pancreas 1998; 16: 312–315. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

