Polypoidal choroidal vasculopathy treated with macular translocation: clinical pathological correlation
- PMID: 11864892
- PMCID: PMC1771039
- DOI: 10.1136/bjo.86.3.321
Polypoidal choroidal vasculopathy treated with macular translocation: clinical pathological correlation
Abstract
Aims: To report the histopathology of two specimens of polypoidal choroidal vasculopathy (PCV) obtained from two eyes of Japanese patients.
Methods: Specimens were obtained under direct visualisation during macular translocation surgery with 360 degree retinotomy. The clinical findings were correlated with the light microscopic findings of the two specimens.
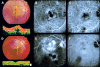
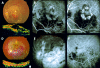
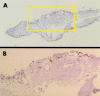
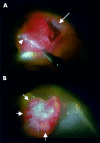
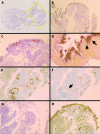
Results: One specimen from a 77 year old man was the central portion of the lesion that lay under the sensory retina on the retinal pigment epithelium (RPE). The specimen was made up mainly of fibrous tissue with small, thin walled vessels. Indocyanine green angiography after surgery revealed that active leaking polypoidal element remained under the RPE. Another specimen obtained from a 62 year old man was made up of a fibrovascular membrane situated within Bruch's membrane. The part of this specimen inferior to the foveal region included a collection of dilated, thin walled blood vessels without pericytes, surrounded by macrophages that stained positive for CD68. The dilated vessels appeared to be correlated with the orange coloured polyps observed by ophthalmoscopy, the polypoidal structure seen in indocyanine green angiograms, and the pyramidal elevation with intermediate reflectivity by optical coherence tomography.
Conclusion: Polypoidal structures are located within Bruch's space. They are composed of clusters of dilated, thin walled blood vessels surrounded by macrophages and fibrin material. The positive immunohistochemical staining for vascular endothelial growth factor in the RPE and the vascular endothelial cells suggests that this fibrovascular complex is a subretinal choroidal neovascularisation.
Figures
References
-
- Yannuzzi LA. Idiopathic polypoidal choroidal vasculopathy. Presented at the 1982 Macula Society meeting.
-
- Yannuzzi LA, Sorenson J, Spaide RF, et al. Idiopathic polypoidal choroidal vasculopathy (IPCV). Retina 1990;10:1–8. - PubMed
-
- Stern RM, Zakov ZN, Zegarra H, et al. Multiple recurrent serosanguineous retinal pigment epithelial detachments in black women. Am J Ophthalmol 1985;100:560–9. - PubMed
-
- Perkovich BT, Zakov ZN, Berlin LA, et al. An update on multiple recurrent serosanguineous retinal pigment epithelial detachments in black women. Retina 1990;10:18–26. - PubMed
-
- Kleiner RC, Brucker AJ, Johnston RL. The posterior uveal bleeding syndrome. Retina 1990;10:9–17. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
