Accelerated hyperfractionation (AHF) compared to conventional fractionation (CF) in the postoperative radiotherapy of locally advanced head and neck cancer: influence of proliferation
- PMID: 11870530
- PMCID: PMC2375281
- DOI: 10.1038/sj.bjc.6600119
Accelerated hyperfractionation (AHF) compared to conventional fractionation (CF) in the postoperative radiotherapy of locally advanced head and neck cancer: influence of proliferation
Abstract
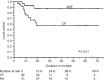
Based on the assumption that an accelerated proliferation process prevails in tumour cell residues after surgery, the possibility that treatment acceleration would offer a therapeutic advantage in postoperative radiotherapy of locally advanced head and neck cancer was investigated. The value of T(pot) in predicting the treatment outcome and in selecting patients for accelerated fractionation was tested. Seventy patients with (T2/N1-N2) or (T3-4/any N) squamous cell carcinoma of the oral cavity, larynx and hypopharynx who underwent radical surgery, were randomized to either (a) accelerated hyperfractionation: 46.2 Gy per 12 days, 1.4 Gy per fraction, three fractions per day with 6 h interfraction interval, treating 6 days per week or (b) Conventional fractionation: 60 Gy per 6 weeks, 2 Gy per fraction, treating 5 days per week. The 3-year locoregional control rate was significantly better in the accelerated hyperfractionation (88 +/- 4%) than in the CF (57+/- 9%) group, P=0.01 (and this was confirmed by multivariate analysis), but the difference in survival (60 +/- 10% vs 46 +/- 9%) was not significant (P=0.29). The favourable influence of a short treatment time was further substantiated by demonstrating the importance of the gap between surgery and radiotherapy and the overall treatment time between surgery and end of radiotherapy. Early mucositis progressed more rapidly and was more severe in the accelerated hyperfractionation group; reflecting a faster rate of dose accumulation. Xerostomia was experienced by all patients with a tendency to be more severe after accelerated hyperfractionation. Fibrosis and oedema also tended to be more frequent after accelerated hyperfractionation and probably represent consequential reactions. T(pot) showed a correlation with disease-free survival in a univariate analysis but did not prove to be an independent factor. Moreover, the use of the minimum and corrected P-values did not identify a significant cut-off. Compared to conventional fractionation, accelerated hyperfractionation did not seem to offer a survival advantage in fast tumours though a better local control rate was noted. This limits the use of T(pot) as a guide for selecting patients for accelerated hyperfractionation. For slowly growing tumours, tumour control and survival probabilities were not significantly different in the conventional fractionation and accelerated hyperfractionation groups. A rapid tumour growth was associated with a higher risk of distant metastases (P=0.01). In conclusion, tumour cell repopulation seems to be an important determinant of postoperative radiotherapy of locally advanced head and neck cancer despite lack of a definite association between T(pot) and treatment outcome. In fast growing tumours accelerated hyperfractionation provided an improved local control but without a survival advantage. To gain a full benefit from treatment acceleration, the surgery-radiotherapy gap and the overall treatment time should not exceed 6 and 10 weeks respectively.
Figures
References
-
- AltmanDGLausenBSauerbreiWSchumacherM1994Dangers of using optimal cutpoints in the evaluation of prognostic factors J Natl Cancer Inst 86429435
-
- AngKKTrottiABrownBWGardenASFooteRLMorrisonWHGearaFBKlotchDWGoepfertHPetersKJ2001Randomized trial addressing risk features and time factors of surgery plus radiotherapy in advanced head and neck cancer Int J Rad Oncol Biol Phys 51571578 - PubMed
-
- AwwadHKKhafagyYBarsoumMEzzatSEl-AttarIFaragHAkoushHMeabidHZaghloulS1992Accelerated versus conventional fractionation in the postoperative irradiation of locally advanced head and neck cancer: influence of tumour proliferation Radiother Oncol 25261266 - PubMed
-
- BeggACHaustermansKHartAAMDischeSSaundersMZackrissonBGustaffsonHCouckePPaschoudNHoyerMOvergaardJAntognoniPRichettiABourhisJBartelinkHHoriotJ-CCorvoRGiarettiWAwwadHShoumanTJouffroyTMaciorowskiZDobrowskyWStruikmansHRoutgersDWilsonGD1999The value of pretreatment cell kinetic parameters as predictors for radiotherapy outcome in head and neck cancer: a multicenter analysis Radiother Oncol 501323 - PubMed
-
- BeggACMcnallyNJShrieveDCKärcherH1985A method to measure duration of DNA synthesis and the potential doubling time from a single sample Cytometry 6620626 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous