Inhibition of leukocyte rolling by nitric oxide during sepsis leads to reduced migration of active microbicidal neutrophils
- PMID: 12065501
- PMCID: PMC128083
- DOI: 10.1128/IAI.70.7.3602-3610.2002
Inhibition of leukocyte rolling by nitric oxide during sepsis leads to reduced migration of active microbicidal neutrophils
Abstract
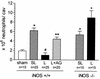
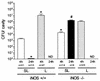
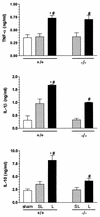
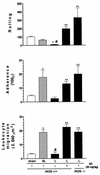
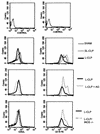
We developed two models of sepsis with different degrees of severity, sublethal and lethal sepsis, induced by cecal ligation and puncture. Lethal sepsis induced by cecal ligation and puncture (L-CLP) resulted in failure of neutrophil migration to the infection site and high mortality. Treatment of septic animals with aminoguanidine (AG), a nitric oxide (NO) synthase inhibitor, precluded the failure of neutrophil migration and protected the animals from death. However, cytokine-induced NO synthase (iNOS)-deficient (iNOS(-/-)) mice subjected to L-CLP did not present neutrophil migration failure, but 100% lethality occurred. iNOS(-/-) mice subjected to sublethal sepsis induced by cecal ligation and puncture (SL-CLP) also suffered high mortality despite the occurrence of neutrophil migration. This apparent paradox could be explained by the lack of microbicidal activity in neutrophils of iNOS(-/-) mice present at the infection site due to their inability to produce NO. Notably, SL- and L-CLP iNOS(-/-) mice showed high bacterial numbers in exudates. The inhibition of neutrophil migration by NO is due to inhibition of a neutrophil/endothelium adhesion mechanism, since a reduction in leukocyte rolling, adhesion, and emigration was observed in L-CLP wild-type mice. These responses were prevented by AG treatment and were not observed in the iNOS(-/-) L-CLP group. There was no significant change in L-selectin expression in neutrophils from L-CLP mice. Thus, it seems that the decrease in leukocyte rolling is due to a defect in the expression of adhesion molecules on endothelial surfaces mediated by iNOS-derived NO. In conclusion, the results indicate that despite the importance of NO in neutrophil microbicidal activity, its generation in severe sepsis reduces neutrophil migration by inhibiting leukocyte rolling and their firm adhesion to the endothelium, in effect impairing the migration of leukocytes and consequently their fundamental role in host cell defense mechanisms.
Figures
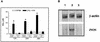
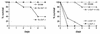
References
-
- Astiz, M. E., and E. C. Rackow. 1998. Septic shock. Lancet 351:1501-1505. - PubMed
-
- Baez, S. 1969. Simultaneous measurements of radii and wall thickness of microvessels in the anesthetized rat. Circ. Res. 25:315-329. - PubMed
-
- Bagby, G. J., K. J. Plessala, L. A. Wilson, J. J. Thompson, and S. Nelson. 1991. Divergent efficacy of antibody to tumor necrosis factor-α in intravascular and peritonitis models of sepsis. J. Infect. Dis. 163:83-88. - PubMed
-
- Baker, C. C., I. H. Chaudry, H. O. Gaines, and A. E. Bauer. 1983. Evaluation of factors affecting mortality rate after sepsis in a murine cecal ligation and puncture model. Surgery 94:331-335. - PubMed
-
- Benjamim, C. F., S. H. Ferreira, and F. Q. Cunha. 2000. Role of nitric oxide in the failure of neutrophil migration in sepsis. J. Infect. Dis. 182:214-223. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

