Guanylate-binding protein-1 expression is selectively induced by inflammatory cytokines and is an activation marker of endothelial cells during inflammatory diseases
- PMID: 12414522
- PMCID: PMC1850787
- DOI: 10.1016/S0002-9440(10)64452-5
Guanylate-binding protein-1 expression is selectively induced by inflammatory cytokines and is an activation marker of endothelial cells during inflammatory diseases
Abstract
During angiogenesis and inflammatory processes, endothelial cells acquire different activation phenotypes, whose identification may help in understanding the complex network of angiogenic and inflammatory interactions in vivo. To this goal we investigated the expression of the human guanylate-binding protein (GBP)-1 that is highly induced by inflammatory cytokines (ICs) and, therefore, may characterize IC-activated cells. Using a new rat monoclonal antibody raised against GBP-1, we show that GBP-1 is a cytoplasmic protein and that its expression in endothelial cells is selectively induced by interferon-gamma, interleukin-1alpha, interleukin-1beta, or tumor necrosis factor-alpha, but not by other cytokines, chemokines, or growth factors. Moreover, we found that GBP-1 expression is highly associated with vascular endothelial cells as confirmed by the simultaneous detection of GBP-1 and the endothelial cell-associated marker CD31 in a broad range of human tissues. Notably, GBP-1 expression was undetectable in the skin, but it was highly induced in vessels of skin diseases with a high-inflammatory component including psoriasis, adverse drug reactions, and Kaposi's sarcoma. These results indicate that GBP-1 is a novel cellular activation marker that characterizes the IC-activated phenotype of endothelial cells.
Figures

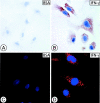



References
-
- Cines DB, Pollak ES, Buck CA, Loscalzo J, Zimmerman GA, McEver RP, Pober JS, Wick TM, Konkle BA, Schwartz BS, Barnathan ES, McCrae KR, Hug BA, Schmidt AM, Stern DM: Endothelial cells in physiology and in the pathophysiology of vascular disorders. Blood 1998, 91:3527-3561 - PubMed
-
- Cotran RS, Pober JS: Endothelial Activation: Its Role in Inflammatory and Immune Reactions. 1988:pp 335-347 Plenum Press, New York
-
- Roesen P, Ferber P, Tschoepe D: Macrovascular disease in diabetes: current status. Exp Clin Endocrinol Diabetes 2001, 109(Suppl):S474-S486 - PubMed
-
- Baumgartl HJ, Standl E: The atherosclerotic process and its exacerbation by diabetes. Exp Clin Endocrinol Diabetes 2001, 109(Suppl):S487-S492 - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

