How could pathologists improve the initial diagnosis of colitis? Evidence from an international workshop
- PMID: 12461067
- PMCID: PMC1769831
- DOI: 10.1136/jcp.55.12.955
How could pathologists improve the initial diagnosis of colitis? Evidence from an international workshop
Abstract
Background: The taking of multiple colorectal biopsies is in widespread use although there is little research into their benefit for the pathological diagnosis of inflammatory bowel disease. There is also still debate about appropriate morphological criteria for interpreting these biopsies.
Aims: To determine the effect of single versus multiple biopsies on the accuracy of diagnosis and to study the accuracy and reproducibility of the different criteria used in the diagnosis of multiple biopsies by expert and non-expert pathologists.
Method: Thirteen expert and 12 non-expert international diagnostic histopathologists attended a workshop. Sixty cases with full follow up were viewed, blinded, in two rounds. Diagnoses were made on rectal biopsies and then full colonoscopic series.
Results: Experts correctly identified 24% of Crohn's disease cases (non-experts, 12%) from the rectal biopsies. This improved to 64% (non-experts, 60%) with the full series. The accuracy of the diagnosis of ulcerative colitis also improved slightly with the full series from 64% to 74% overall. Experts had a similar (moderate) level of agreement and accuracy to non-experts. For Crohn's disease, the likelihood ratios (LR) for the most important individual features were 12.4 for granulomas and 3.3 for focal or patchy inflammation. Features favouring ulcerative colitis were diffuse crypt architectural irregularity (LR, 3.4), general crypt epithelial polymorphs (LR, 3.7), and reduced crypt numbers (LR, 2.9).
Conclusions: A full colonoscopic series gave more accurate diagnosis than a rectal biopsy. Accurate pathologists used the same evidence based criteria for multiple biopsies as for single biopsies.
Figures
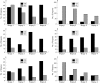
Comment in
-
Endoscopic biopsies.J Clin Pathol. 2003 May;56(5):321-2. doi: 10.1136/jcp.56.5.321. J Clin Pathol. 2003. PMID: 12719448 Free PMC article. No abstract available.
References
-
- Geboes K, Ectors N, D’Haens G, et al. Is ileoscopy with biopsy worthwhile in patients presenting with symptoms of inflammatory bowel disease? Am J Gastroenterol 1998;93:201–6. - PubMed
-
- Dundas SA, Dutton J, Skipworth P. Reliability of rectal biopsy in distinguishing between chronic inflammatory bowel disease and acute self-limiting colitis. Histopathology 1997;31:60–6. - PubMed
-
- Tanaka M, Riddell RH, Saito H, et al. Morphologic criteria applicable to biopsy specimens for effective distinction of inflammatory bowel disease from other forms of colitis and of Crohn’s disease from ulcerative colitis. Scand J Gastroenterol 1999;34:55–67. - PubMed
-
- Tobin JM, Sinha B, Ramani P, et al. Upper gastrointestinal mucosal disease in pediatric Crohn disease and ulcerative colitis: a blinded, controlled study. J Pediatr Gastroenterol Nutr 2001;32:443–8. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
