Radiofrequency ablation of adrenal tumors and adrenocortical carcinoma metastases
- PMID: 12548596
- PMCID: PMC2443414
- DOI: 10.1002/cncr.11084
Radiofrequency ablation of adrenal tumors and adrenocortical carcinoma metastases
Abstract
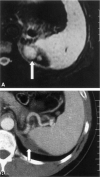
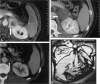
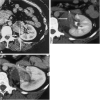
Background: The current study was performed to analyze the feasibility, safety, imaging appearance, and short-term efficacy of image-guided percutaneous radiofrequency ablation (RFA) of primary and metastatic adrenal neoplasms including adrenocortical carcinoma.
Methods: The procedure was performed using 36 treatment spheres on 15 adrenocortical carcinoma primary or metastatic tumors in eight patients over 27 months. Tumors ranged from 15 to 90 mm in greatest dimension with a mean of 43 mm. All patients had unresectable tumors or were poor candidates for surgery. Mean follow-up was 10.3 months.
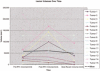
Results: All patients were discharged or were free of procedure-related medical care 6-48 hours after the procedures without major complications. All treatments resulted in presumptive coagulation necrosis by imaging criteria, which manifested as loss of previous contrast enhancement in ablated tissue. Eight of 15 (53%) posttreatment thermal lesions lost enhancement and stopped growing on latest follow-up computed tomographic scan. Three of 15 (20%) demonstrated interval growth and four did not change in size. Of these four lesions, two showed contrast enhancement. For smaller tumors with a mean greatest dimension less than or equal to 5 cm, 8 of 12 (67%) tumors were completely ablated, as defined by decreasing size and complete loss of contrast enhancement. Three of 15 (20 %) tumors and related thermal lesions were found to have disappeared nearly completely on imaging.
Conclusions: Percutaneous, image-guided RFA is a safe and well tolerated procedure for the treatment of unresectable primary or metastatic adrenocortical carcinoma. The procedure is effective for the short-term local control of small adrenal tumors, and is most effective for tumors less than 5 cm. The survival rate for patients with adrenocortical carcinoma improves when radical excision is performed in selected patients. Aggressive local disease control may potentially influence survival as well. However, further study is required to evaluate survival impact, document long-term efficacy, and to determine if RFA can obviate repeated surgical intervention in specific clinical scenarios.
Figures
References
-
- Demeure MJ, Somberg LB. Functioning and nonfunctioning adrenocortical carcinoma. Surg Oncol Clin North Am. 1998;7:791–805. - PubMed
-
- Luton JP, Cerdas S, Billaud L, et al. Clinical features of adrenocortical carcinoma, prognostic factors and the effect of mitotane therapy. N Engl J Med. 1990;332:1195–1201. - PubMed
-
- Vassilopoulou-Sellin R, Guinee VF, Klein MJ, et al. Impact of adjuvant mitotane on the clinical course of patients with adrenocortical cancer. Cancer. 1993;71:3119–3123. - PubMed
-
- Decker RA, Elson P, Hogan TF, et al. Eastern Cooperative Oncology Group study 1879: mitotane and Adriamycin in patients with advanced adrenocrtical carcinoma. Surgery. 1991;110:1006–1013. - PubMed
-
- Bukowski RM, Wolfe M, Levine HS, et al. Phase II trial of mitotane and cisplatin in patients with adrenal carcinoma: a Southwest Oncology Group Study. J Clin Oncol. 1993;11:161–165. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

