Dissociation by steroids of eosinophilic inflammation from airway hyperresponsiveness in murine airways
- PMID: 12657158
- PMCID: PMC152648
- DOI: 10.1186/rr197
Dissociation by steroids of eosinophilic inflammation from airway hyperresponsiveness in murine airways
Abstract
Background: The link between eosinophils and the development of airway hyperresponsiveness (AHR) in asthma is still controversial. This question was assessed in a murine model of asthma in which we performed a dose ranging study to establish whether the dose of steroid needed to inhibit the eosinophil infiltration correlated with that needed to block AHR.
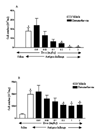
Methods: The sensitised BALB/c mice were dosed with vehicle or dexamethasone (0.01-3 mg/kg) 2 hours before and 6 hours after each challenge (once daily for 6 days) and 2 hours before AHR determination by whole-body plethysmography. At 30 minutes after the AHR to aerosolised methacholine the mice were lavaged and differential white cell counts were determined. Challenging with antigen caused a significant increase in eosinophils in the bronchoalveolar lavage (BAL) fluid and lung tissue, and increased AHR.
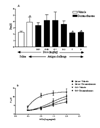
Results: Dexamethasone reduced BAL and lung tissue eosinophilia (ED50 values of 0.06 and 0.08 mg/kg, respectively), whereas a higher dose was needed to block AHR (ED50 of 0.32 mg/kg at 3 mg/ml methacholine. Dissociation was observed between the dose of steroid needed to affect AHR in comparison with eosinophilia and suggests that AHR is not a direct consequence of eosinophilia.
Conclusion: This novel pharmacological approach has revealed a clear dissociation between eosinophilia and AHR by using steroids that are the mainstay of asthma therapy. These data suggest that eosinophilia is not associated with AHR and questions the rationale that many pharmaceutical companies are adopting in developing low-molecular-mass compounds that target eosinophil activation/recruitment for the treatment of asthma.
Figures
Similar articles
-
Modulation of airway hyperresponsiveness and eosinophilia by selective histamine and 5-HT receptor antagonists in a mouse model of allergic asthma.Br J Pharmacol. 1998 Jul;124(5):857-64. doi: 10.1038/sj.bjp.0701901. Br J Pharmacol. 1998. PMID: 9692769 Free PMC article.
-
TRFK-5 reverses established airway eosinophilia but not established hyperresponsiveness in a murine model of chronic asthma.Am J Respir Crit Care Med. 1999 Feb;159(2):580-7. doi: 10.1164/ajrccm.159.2.9712018. Am J Respir Crit Care Med. 1999. PMID: 9927376
-
Effect of suplatast tosilate (IPD-1151T) on a mouse model of asthma: inhibition of eosinophilic inflammation and bronchial hyperresponsiveness.Int Arch Allergy Immunol. 2000 Feb;121(2):116-22. doi: 10.1159/000024306. Int Arch Allergy Immunol. 2000. PMID: 10705221
-
Cessation of dexamethasone exacerbates airway responses to methacholine in asthmatic mice.Eur J Pharmacol. 2007 Jun 1;563(1-3):213-5. doi: 10.1016/j.ejphar.2007.02.028. Epub 2007 Feb 23. Eur J Pharmacol. 2007. PMID: 17374534
-
Vbeta8+ T lymphocytes are essential in the regulation of airway hyperresponsiveness and bronchoalveolar eosinophilia but not in allergen-specific IgE in a murine model of allergic asthma.Clin Exp Allergy. 1998 Dec;28(12):1571-80. doi: 10.1046/j.1365-2222.1998.00387.x. Clin Exp Allergy. 1998. PMID: 10024230
Cited by
-
Dysregulation of alveolar macrophages unleashes dendritic cell-mediated mechanisms of allergic airway inflammation.Mucosal Immunol. 2014 Jan;7(1):155-64. doi: 10.1038/mi.2013.34. Epub 2013 May 29. Mucosal Immunol. 2014. PMID: 23715174
-
Antigen-sensitized CD4+CD62Llow memory/effector T helper 2 cells can induce airway hyperresponsiveness in an antigen free setting.Respir Res. 2005 May 28;6(1):46. doi: 10.1186/1465-9921-6-46. Respir Res. 2005. PMID: 15921525 Free PMC article.
-
Adjustment of sensitisation and challenge protocols restores functional and inflammatory responses to ovalbumin in guinea-pigs.J Pharmacol Toxicol Methods. 2015 Mar-Apr;72:85-93. doi: 10.1016/j.vascn.2014.10.007. Epub 2014 Oct 30. J Pharmacol Toxicol Methods. 2015. PMID: 25450500 Free PMC article.
-
Respiratory infections cause the release of extracellular vesicles: implications in exacerbation of asthma/COPD.PLoS One. 2014 Jun 27;9(6):e101087. doi: 10.1371/journal.pone.0101087. eCollection 2014. PLoS One. 2014. PMID: 24972036 Free PMC article.
-
Different effects of acetyl-CoA carboxylase inhibitor TOFA on airway inflammation and airway resistance in a mice model of asthma.Pharmacol Rep. 2020 Aug;72(4):1011-1020. doi: 10.1007/s43440-019-00027-8. Epub 2020 Jan 8. Pharmacol Rep. 2020. PMID: 32048254 Free PMC article.
References
-
- Brusasco V, Crimi E, Gianiorio P, Lantero S, Rossi GA. Allergen-induced increase in airway responsiveness and inflammation in mild asthma. J Appl Physiol. 1990;69:2209–2214. - PubMed
-
- Wanner A, Abraham WM, Douglas JS, Drazen JM, Richerson HB, Ram JS. NHLBI Workshop Summary. Models of airway hyperresponsiveness. Am Rev Respir Dis. 1990;141:253–257. - PubMed
-
- Kirby JG, Hargreave FE, Gleich GJ, O'Byrne PM. Bronchoalveolar cell profiles of asthmatic and nonasthmatic subjects. Am Rev Respir Dis. 1987;136:379–383. - PubMed
-
- Bradley BL, Azzawi M, Jacobson M, Assoufi B, Collins JV, Irani AM, Schwartz LB, Durham SR, Jeffery PK, Kay AB. Eosinophils, T-lymphocytes, mast cells, neutrophils, and macrophages in bronchial biopsy specimens from atopic subjects with asthma: comparison with biopsy specimens from atopic subjects without asthma and normal control subjects and relationship to bronchial hyperresponsiveness. J Allergy Clin Immunol. 1991;88:661–674. - PubMed
-
- Battram C, Birrell M, Foster M, Webber SE, Belvisi MG. Comparison of inhaled spasmogen as determinants of airway hyperresponsiveness in a murine model of asthma. Br J Pharmacol. 1999;128:271P.

