CD28-dependent Rac1 activation is the molecular target of azathioprine in primary human CD4+ T lymphocytes
- PMID: 12697733
- PMCID: PMC152932
- DOI: 10.1172/JCI16432
CD28-dependent Rac1 activation is the molecular target of azathioprine in primary human CD4+ T lymphocytes
Abstract
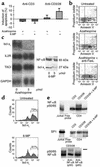
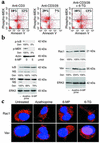
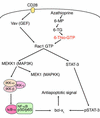
Azathioprine and its metabolite 6-mercaptopurine (6-MP) are immunosuppressive drugs that are used in organ transplantation and autoimmune and chronic inflammatory diseases such as Crohn disease. However, their molecular mechanism of action is unknown. In the present study, we have identified a unique and unexpected role for azathioprine and its metabolites in the control of T cell apoptosis by modulation of Rac1 activation upon CD28 costimulation. We found that azathioprine and its metabolites induced apoptosis of T cells from patients with Crohn disease and control patients. Apoptosis induction required costimulation with CD28 and was mediated by specific blockade of Rac1 activation through binding of azathioprine-generated 6-thioguanine triphosphate (6-Thio-GTP) to Rac1 instead of GTP. The activation of Rac1 target genes such as mitogen-activated protein kinase kinase (MEK), NF-kappaB, and bcl-x(L) was suppressed by azathioprine, leading to a mitochondrial pathway of apoptosis. Azathioprine thus converts a costimulatory signal into an apoptotic signal by modulating Rac1 activity. These findings explain the immunosuppressive effects of azathioprine and suggest that 6-Thio-GTP derivates may be useful as potent immunosuppressive agents in autoimmune diseases and organ transplantation.
Figures




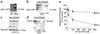
Comment in
-
Azathioprine: old drug, new actions.J Clin Invest. 2003 Apr;111(8):1122-4. doi: 10.1172/JCI18384. J Clin Invest. 2003. PMID: 12697731 Free PMC article. No abstract available.
References
-
- McGeown M, et al. Ten-year results of renal transplantation with azathioprine and prednisolone as only immunosuppression. Lancet. 1988;1:983–991. - PubMed
-
- Andreone PA, et al. Reduction of infectious complications following heart transplantation with triple-drug immunotherapy. J. Heart Transplant. 1986;5:13–19. - PubMed
-
- BritishDutch Multiple Sclerosis Azathioprine Trial Group. Double-masked trial of azathioprine in multiple sclerosis. Lancet. 1988;2:179–186. - PubMed
-
- Ginzler E, Sharon E, Diamond H, Kaplan D. Long term maintenance therapy with azathioprine in systemic lupus erythematosus. Arthritis Rheum. 1975;18:27–35. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases
Research Materials
Miscellaneous

