Urokinase, a constitutive component of the inflamed synovial fluid, induces arthritis
- PMID: 12716448
- PMCID: PMC154426
- DOI: 10.1186/ar606
Urokinase, a constitutive component of the inflamed synovial fluid, induces arthritis
Abstract
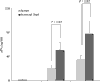
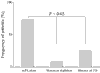
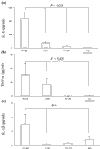
Urokinase plasminogen activator (uPA) is an important regulator of fibrinolysis in synovial fluid. An increase of uPA activity and expression of its receptor have been reported in joints of patients with rheumatoid arthritis (RA). The aim of the present study was to assess the arthritogenic capacity of uPA and the mechanisms by which this effect is mediated. uPA was injected into the knee joints of healthy mice, and morphological signs of arthritis were assessed 4 days after the injection. The prerequisite of different leukocyte populations for the development of uPA-triggered arthritis was assessed by selective cell depletion. The inflammatory capacity of uPA was assessed in vitro. Finally, levels of uPA were measured in 67 paired blood and synovial fluid samples from RA patients. The synovial fluid from RA patients displayed higher levels of uPA compared with blood samples. Morphological signs of arthritis were found in 72% of uPA-injected joints compared with in only 18% of joints injected with PBS (P < 0.05). Synovitis was characterised by infiltration of CD4-Mac-1+ mononuclear cells, by the formation of pannus and by occasional cartilage destruction. The absence of monocytes and lymphocytes diminished the frequency of synovitis (P < 0.01), indicating an arthritogenic role of both these leukocyte populations. Synthetic uPA inhibitor downregulated the incidence of uPA-triggered arthritis by 50%. uPA induced arthritis, stimulating the release of proinflammatory cytokines IL-6, IL-1beta and tumour necrosis factor alpha. Accumulation of uPA locally in the joint cavity is a typical finding in erosive RA. uPA exerts potent arthritogenic properties and thus may be viewed as one of the essential mediators of joint inflammation.
Figures


References
-
- Weinberg JB, Wortham TS, Misukonis MA, Patton KL, Chitneni SR. Synovial mononuclear phagocytes in rheumatoid arthritis and osteoarthritis: quantitative and functional aspects. Immunol Invest. 1993;22:365–374. - PubMed
-
- Del Rosso M, Fibbi G, Matucci Cerinic M. The urokinase-type plasminogen activator system and inflammatory joint diseases. Clin Exp Rheumatol. 1999;17:485–498. - PubMed
-
- Kummer JA, Abbink JJ, de Boer JP, Roem D, Nieuwenhuys EJ, Kamp AM, Swaak TJ, Hack CE. Analysis of intraarticular fibrinolytic pathways in patients with inflammatory and noninflammatory joint diseases. Arthritis Rheum. 1992;35:884–893. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

