Biologic predictors of survival in node-negative gastric cancer
- PMID: 12796579
- PMCID: PMC1514693
- DOI: 10.1097/01.SLA.0000072260.77776.39
Biologic predictors of survival in node-negative gastric cancer
Abstract
Objective: To evaluate factors predictive of survival following curative resection for node-negative gastric adenocarcinoma.
Summary background data: Presence or absence of lymph node metastases is the most powerful predictor of survival following curative resection for gastric adenocarcinoma. Factors predictive of survival in node-negative gastric cancer have not been clarified.
Methods: Histopathology and clinical outcome for all patients undergoing R0 resections for gastric adenocarcinoma at a tertiary center between 1985 and 2001 were reviewed.
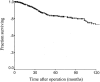
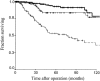
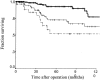
Results: Of 1,256 R0 resections performed, 507 (40%) were node-negative, 465 were T1-T3, and 317 of these were adequately staged, as defined by histologic evaluation of at least 15 lymph nodes. Median age was 67 years, and 62% were male. Forty percent had T1 tumors, 34% were T2, and 26% were T3. Median tumor size was 3 cm. Vascular invasion (VI) was present in 17% of tumors and neural invasion (NI) in 31%. Extended (D2) lymphadenectomy was performed in 75% of cases. Five- and 10-year disease-specific survival rates were 79% and 67% respectively. Factors associated with poorer disease-specific survival on univariate analysis were male gender, serosal invasion, presence of VI, presence of NI, and resection other than distal subtotal gastrectomy. On multivariate analysis, NI was not an independent predictor of survival, but correlated directly with advancing T stage and tumor size.
Conclusions: Serosal invasion and presence of VI are strong predictors of poor survival in this disease. NI correlates with T stage and tumor size and may serve as a marker of advanced disease.
Figures

Similar articles
-
The effect of extended lymphadenectomy on survival in patients with gastric adenocarcinoma.J Am Coll Surg. 1995 Jul;181(1):56-64. J Am Coll Surg. 1995. PMID: 7599772
-
Adenocarcinoma in the middle third of the stomach--an evaluation for the prognostic significance of clinicopathological features.Hepatogastroenterology. 1997 Sep-Oct;44(17):1488-94. Hepatogastroenterology. 1997. PMID: 9356878
-
Does extended lymphadenectomy influence prognosis of gastric carcinoma after curative resection?Hepatogastroenterology. 2000 Sep-Oct;47(35):1470-4. Hepatogastroenterology. 2000. PMID: 11100379
-
Multivariate prognostic study on large gastric cancer.J Surg Oncol. 2007 Jul 1;96(1):14-8. doi: 10.1002/jso.20631. J Surg Oncol. 2007. PMID: 17582596 Review.
-
[Diagnosis of and therapy for gastric cancer--work-flow].Zentralbl Chir. 2009 Aug;134(4):362-74. doi: 10.1055/s-0029-1224534. Epub 2009 Aug 17. Zentralbl Chir. 2009. PMID: 19688686 Review. German.
Cited by
-
Efficacy of Lymph Node Location-Number Hybrid Staging System on the Prognosis of Gastric Cancer Patients.Cancers (Basel). 2023 May 8;15(9):2659. doi: 10.3390/cancers15092659. Cancers (Basel). 2023. PMID: 37174124 Free PMC article.
-
Prediction of liver metastases after gastric cancer resection with the use of learning vector quantization neural networks.Dig Dis Sci. 2010 Nov;55(11):3252-61. doi: 10.1007/s10620-010-1155-z. Epub 2010 Feb 26. Dig Dis Sci. 2010. PMID: 20186483
-
Gastric adenocarcinoma: review and considerations for future directions.Ann Surg. 2005 Jan;241(1):27-39. doi: 10.1097/01.sla.0000149300.28588.23. Ann Surg. 2005. PMID: 15621988 Free PMC article. Review.
-
Prognostic factors in patients with node-negative gastric cancer: an Indian experience.World J Surg Oncol. 2011 May 10;9:48. doi: 10.1186/1477-7819-9-48. World J Surg Oncol. 2011. PMID: 21554745 Free PMC article.
-
Relationship between 15-hydroxyprostaglandin dehydrogenase and gastric adenocarcinoma.Ann Surg Treat Res. 2014 Jun;86(6):302-8. doi: 10.4174/astr.2014.86.6.302. Epub 2014 May 23. Ann Surg Treat Res. 2014. PMID: 24949321 Free PMC article.
References
-
- Shiu MH, Perrotti M, Brennan MF. Adenocarcinoma of the stomach: a multivariate analysis of clinical, pathologic and treatment factors. Hepato-Gastroenterology. 1989; 36: 7–12. - PubMed
-
- Bozzetti F, Bonfanti G, Morabito A, et al. A multifactorial approach for the prognosis of patients with carcinoma of the stomach after curative resection. Surg Gynecol Obstet. 1986; 162: 229–234. - PubMed
-
- Kim JP, Kim YW, Yang HK, et al. Significant prognostic factors by multivariate analysis of 3926 gastric cancer patients. World J Surg. 1994; 18: 872–877. - PubMed
-
- AJCC Cancer Staging Manual. Chicago: Lippincott-Raven, 1997.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

