Chronic submasseteric abscess: anatomic, radiologic, and pathologic features
- PMID: 12812946
- PMCID: PMC8149006
Chronic submasseteric abscess: anatomic, radiologic, and pathologic features
Abstract
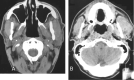
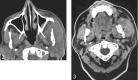
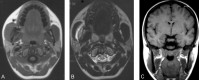
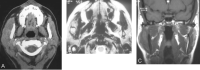
Herein we present five cases of submasseteric abscess that most commonly occurred in patients with a history dental disease. CT has been the main imaging method for diagnosing lesions in the masticator space and adjacent to the mandible; however, we found that, in some of our cases, CT defined the lesion poorly or not at all. In some cases, MR imaging defined the lesion better. Radiologic manifestations of this condition and pathologic correlations are discussed.
Figures

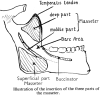
Similar articles
-
[The submasseteric abscess as a complication of the semi-impacted wisdom tooth infection].Hell Period Stomat Gnathopathoprosopike Cheir. 1989 Dec;4(4):191-4. Hell Period Stomat Gnathopathoprosopike Cheir. 1989. PMID: 2640669 Greek, Modern.
-
Diagnosis and surgical treatment of periapical infection of the third mandibular molar in five horses.J Am Vet Med Assoc. 1999 Sep 15;215(6):829-32, 796. J Am Vet Med Assoc. 1999. PMID: 10496139
-
Chronic dental infections mimicking temporomandibular disorders.Aust Dent J. 2002 Mar;47(1):63-5. doi: 10.1111/j.1834-7819.2002.tb00305.x. Aust Dent J. 2002. PMID: 12035960
-
Submasseteric abscess caused by a dentigerous cyst mimicking a parotitis: report of two cases.J Oral Maxillofac Surg. 1997 Sep;55(9):996-9. doi: 10.1016/s0278-2391(97)90077-x. J Oral Maxillofac Surg. 1997. PMID: 9294513 Review. No abstract available.
-
Rapid, early-onset group a streptococcus infection after impacted third molar removal: a review and case series.J Oral Maxillofac Surg. 2012 Dec;70(12):2742-7. doi: 10.1016/j.joms.2012.07.045. Epub 2012 Sep 22. J Oral Maxillofac Surg. 2012. PMID: 23010371 Review. No abstract available.
Cited by
-
Masticator space abscess derived from odontogenic infection: imaging manifestation and pathways of extension depicted by CT and MR in 30 patients.Eur Radiol. 2008 Sep;18(9):1972-9. doi: 10.1007/s00330-008-0946-5. Epub 2008 Apr 17. Eur Radiol. 2008. PMID: 18418606
-
Diagnostic difficulties in a patient with multiple sclerosis who presents with cranial nerve palsies: an unusual complication of dental work.BMJ Case Rep. 2020 Oct 30;13(10):e232903. doi: 10.1136/bcr-2019-232903. BMJ Case Rep. 2020. PMID: 33127721 Free PMC article.
-
Submasseteric abscess caused by Mycoplasma salivarium infection.J Clin Microbiol. 2008 Nov;46(11):3860-2. doi: 10.1128/JCM.00807-08. Epub 2008 Aug 27. J Clin Microbiol. 2008. PMID: 18753349 Free PMC article.
-
The masticator space. Value of computed tomography and magnetic resonance imaging in localisation and characterisation of lesions.Acta Otorhinolaryngol Ital. 2010 Apr;30(2):94-9. Acta Otorhinolaryngol Ital. 2010. PMID: 20559479 Free PMC article.
-
Bisphosphonate therapy and osteonecrosis of the jaw complicated with a temporal abscess in an elderly woman with rheumatoid arthritis: a case report.Clin Interv Aging. 2014 Aug 25;9:1409-13. doi: 10.2147/CIA.S67726. eCollection 2014. Clin Interv Aging. 2014. PMID: 25187700 Free PMC article.
References
-
- Bransby-Zachary GM. The sub-masseteric space. Br Dent J 1948;84:10–13 - PubMed
-
- Tryhus MR, Smoker WR, Harnsberger HR. The normal and diseased masticator space. Semin Ultrasound CT MR 1990;11:476–485 - PubMed
-
- Nyberg DA, Jeffrey RB, Brant-Zawadzki M, et al. Computed tomography of cervical infections. J Comput Assist Tomogr 1985;9:288–296 - PubMed
-
- Kay LW, Killey HC. The surgical problem of the submasseteric abscess. Br J Oral Surg 1963;66:55–62 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
