Near-wall micro-PIV reveals a hydrodynamically relevant endothelial surface layer in venules in vivo
- PMID: 12829517
- PMCID: PMC1303118
- DOI: 10.1016/s0006-3495(03)74507-x
Near-wall micro-PIV reveals a hydrodynamically relevant endothelial surface layer in venules in vivo
Abstract
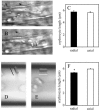
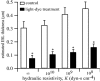
High-resolution near-wall fluorescent microparticle image velocimetry (micro-PIV) was used in mouse cremaster muscle venules in vivo to measure velocity profiles in the red cell-depleted plasma layer near the endothelial lining. micro-PIV data of the instantaneous translational speeds and radial positions of fluorescently labeled microspheres (0.47 microm) in an optical section through the midsagittal plane of each vessel were used to determine fluid particle translational speeds. Regression of a linear velocity distribution based on near-wall fluid-particle speeds consistently revealed a negative intercept when extrapolated to the vessel wall. Based on a detailed three-dimensional analysis of the local fluid dynamics, we estimate a mean effective thickness of approximately 0.33 micro m for an impermeable endothelial surface layer or approximately 0.44 micro m assuming the lowest hydraulic resistivity of the layer that is consistent with the observed particle motions. The extent of plasma flow retardation through the layer required to be consistent with our micro-PIV data results in near complete attenuation of fluid shear stress on the endothelial-cell surface. These findings confirm the presence of a hydrodynamically effective endothelial surface layer, and emphasize the need to revise previous concepts of leukocyte adhesion, stress transmission to vascular endothelium, permeability, and mechanotransduction mechanisms.
Figures

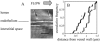
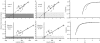
Similar articles
-
The recovery time course of the endothelial cell glycocalyx in vivo and its implications in vitro.Circ Res. 2009 Jun 5;104(11):1318-25. doi: 10.1161/CIRCRESAHA.108.191585. Epub 2009 May 14. Circ Res. 2009. PMID: 19443840 Free PMC article.
-
The hydrodynamically relevant endothelial cell glycocalyx observed in vivo is absent in vitro.Circ Res. 2008 Apr 11;102(7):770-6. doi: 10.1161/CIRCRESAHA.107.160226. Epub 2008 Feb 7. Circ Res. 2008. PMID: 18258858
-
The effect of hematocrit and leukocyte adherence on flow direction in the microcirculation.Ann Biomed Eng. 2004 Jun;32(6):803-14. doi: 10.1023/b:abme.0000030256.37022.02. Ann Biomed Eng. 2004. PMID: 15255211
-
The cytoskeleton under external fluid mechanical forces: hemodynamic forces acting on the endothelium.Ann Biomed Eng. 2002 Mar;30(3):284-96. doi: 10.1114/1.1467926. Ann Biomed Eng. 2002. PMID: 12051614 Review.
-
Rheological effects of red blood cell aggregation in the venous network: a review of recent studies.Biorheology. 2001;38(2-3):263-74. Biorheology. 2001. PMID: 11381180 Review.
Cited by
-
The Biomechanical Effects of Resuscitation Colloids on the Compromised Lung Endothelial Glycocalyx.Anesth Analg. 2016 Aug;123(2):382-93. doi: 10.1213/ANE.0000000000001284. Anesth Analg. 2016. PMID: 27331777 Free PMC article.
-
Effect of erythrocyte aggregation and flow rate on cell-free layer formation in arterioles.Am J Physiol Heart Circ Physiol. 2010 Jun;298(6):H1870-8. doi: 10.1152/ajpheart.01182.2009. Epub 2010 Mar 26. Am J Physiol Heart Circ Physiol. 2010. PMID: 20348228 Free PMC article.
-
Singular perturbation theory for predicting extravasation of Brownian particles.J Eng Math. 2014 Feb 1;84(1):155-171. doi: 10.1007/s10665-013-9665-2. J Eng Math. 2014. PMID: 24563548 Free PMC article.
-
Tuning the formation and rupture of single ligand-receptor bonds by hyaluronan-induced repulsion.Biophys J. 2008 Oct;95(8):3999-4012. doi: 10.1529/biophysj.108.135947. Epub 2008 Jul 3. Biophys J. 2008. PMID: 18599637 Free PMC article.
-
Measurements of the wall shear stress distribution in the outflow tract of an embryonic chicken heart.J R Soc Interface. 2010 Jan 6;7(42):91-103. doi: 10.1098/rsif.2009.0063. Epub 2009 Apr 28. J R Soc Interface. 2010. PMID: 19401309 Free PMC article.
References
-
- Baez, S. 1973. An open cremaster muscle preparation for the study of blood vessels by in vivo microscopy. Microvasc. Res. 5:384–394. - PubMed
-
- Cokelet, G. R. 1999. Viscometric, in vitro and in vivo blood viscosity relationships: how are they related? Biorheology. 36:343–358. - PubMed
-
- Damiano, E. R. 1998a. Blood flow in microvessels lined with a poroelastic wall layer. In Poromechanics. J.-F. Thimus, Y. Abousleiman, A. H. D. Cheng, O. Coussy, and E. Detournay, editors. Balkema, Rotterdam, The Netherlands. 403–408.
-
- Damiano, E. R. 1998b. The effect of the endothelial-cell glycocalyx on the motion of red blood cells through capillaries. Microvasc. Res. 55:77–91. - PubMed
-
- Damiano, E. R., B. R. Duling, K. Ley, and T. C. Skalak. 1996. Axisymmetric pressure-driven flow of rigid pellets through a cylindrical tube lined with a deformable porous wall layer. J. Fluid Mech. 314:163–189.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

