Alterations of intestinal mucosa structure and barrier function following traumatic brain injury in rats
- PMID: 14669332
- PMCID: PMC4612051
- DOI: 10.3748/wjg.v9.i12.2776
Alterations of intestinal mucosa structure and barrier function following traumatic brain injury in rats
Abstract
Aim: Gastrointestinal dysfunction is a common complication in patients with traumatic brain injury (TBI). However, the effect of traumatic brain injury on intestinal mucosa has not been studied previously. The aim of the current study was to explore the alterations of intestinal mucosa morphology and barrier function, and to determine how rapidly the impairment of gut barrier function occurs and how long it persists following traumatic brain injury.
Methods: Male Wistar rats were randomly divided into six groups (6 rats each group) including controls without brain injury and traumatic brain injury groups at hours 3, 12, 24, and 72, and on day 7. The intestinal mucosa structure was detected by histopathological examination and electron microscopy. Gut barrier dysfunction was evaluated by detecting serum endotoxin and intestinal permeability. The level of serum endotoxin and intestinal permeability was measured by using chromogenic limulus amebocyte lysate and lactulose/mannitol (L/M) ratio, respectively.
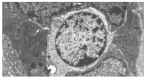
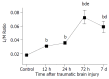
Results: After traumatic brain injury, the histopathological alterations of gut mucosa occurred rapidly as early as 3 hours and progressed to a serious state, including shedding of epithelial cells, fracture of villi, focal ulcer, fusion of adjacent villi, dilation of central chyle duct, mucosal atrophy, and vascular dilation, congestion and edema in the villous interstitium and lamina propria. Apoptosis of epithelial cells, fracture and sparseness of microvilli, loss of tight junction between enterocytes, damage of mitochondria and endoplasm, were found by electron microscopy. The villous height, crypt depth and surface area in jejunum decreased progressively with the time of brain injury. As compared with that of control group (183.7 +/- 41.8 EU/L), serum endotoxin level was significantly increased at 3, 12, and 24 hours following TBI (434.8 +/- 54.9 EU/L, 324.2 +/- 61.7 EU/L and 303.3 +/- 60.2 EU/L, respectively), and peaked at 72 hours (560.5 +/- 76.2 EU/L), then declined on day 7 (306.7 +/- 62.4 EU/L, P<0.01). Two peaks of serum endotoxin level were found at hours 3 and 72 following TBI. L/M ratio was also significantly higher in TBI groups than that in control group (control, 0.0172 +/- 0.0009; 12 h, 0.0303 +/- 0.0013; 24 h, 0.0354 +/- 0.0025; 72 h, 0.0736 +/- 0.0105; 7 d, 0.0588 +/- 0.0083; P<0.01).
Conclusion: Traumatic brain injury can induce significant damages of gut structure and impairment of barrier function which occur rapidly as early as 3 hours following brain injury and lasts for more than 7 days with marked mucosal atrophy.
Figures








References
-
- Pilitsis JG, Rengachary SS. Complications of head injury. Neurol Res. 2001;23:227–236. - PubMed
-
- Lu WY, Rhoney DH, Boling WB, Johnson JD, Smith TC. A review of stress ulcer prophylaxis in the neurosurgical intensive care unit. Neurosurgery. 1997;41:416–25; discussion 425-6. - PubMed
-
- Brown TH, Davidson PF, Larson GM. Acute gastritis occurring within 24 hours of severe head injury. Gastrointest Endosc. 1989;35:37–40. - PubMed
-
- Kamada T, Fusamoto H, Kawano S, Noguchi M, Hiramatsu K. Gastrointestinal bleeding following head injury: a clinical study of 433 cases. J Trauma. 1977;17:44–47. - PubMed
-
- Kao CH, ChangLai SP, Chieng PU, Yen TC. Gastric emptying in head-injured patients. Am J Gastroenterol. 1998;93:1108–1112. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials

