Accelerated regrowth of non-small-cell lung tumours after induction chemotherapy
- PMID: 14676792
- PMCID: PMC2395273
- DOI: 10.1038/sj.bjc.6601418
Accelerated regrowth of non-small-cell lung tumours after induction chemotherapy
Abstract
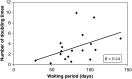
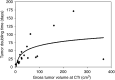
Induction chemotherapy of non-small-cell lung cancer (NSCLC) stage III with gemcitabine and cisplatin for downstaging of the tumour with the aim for further treatment with ionising radiation is one of the treatments for lung cancer patients. The purpose of this study was to investigate the influence of the waiting time for radiotherapy, that is, the interval between induction chemotherapy and radiotherapy, on the rate of tumour growth for patients with NSCLC. Interval times between the end of induction chemotherapy and date of diagnostic CT, planning CT and first day of radiotherapy were determined for 23 patients with NSCLC. Increase in gross tumour volume was measured for 18 patients by measuring the dimensions of the primary tumour and lymph node metastases on the diagnostic CT after induction chemotherapy and on the CT used for radiotherapy planning. For each patient, the volume doubling time was calculated from the time interval between the two CTs and ratio of the gross volumes on planning CT and diagnostic CT. The mean time interval between end of chemotherapy and day of diagnostic CT was 16 days, and till first day of radiotherapy 80.3 (range 29-141) days. In all, 41% of potentially curable patients became incurable in the waiting period. The ratio of gross tumour volumes of the two CTs ranged from 1.1 to 81.8 and the tumour doubling times ranged from 8.3 to 171 days, with a mean value of 46 days and median value of 29 days. This is far less than the mean doubling time of NSCLC in untreated patients found in the literature. This study shows that in the time interval between the end of induction chemotherapy and the start of radiotherapy rapid tumour progression occurs as a result of accelerated tumour cell proliferation: mean tumour doubling times are much shorter than those in not treated tumours. As a consequence, the gain obtained with induction chemotherapy with regard to volume reduction was lost in the waiting time for radiotherapy. We recommend diminishing the time interval between chemo- and radiotherapy to as short as possible.
Figures

References
-
- Abe Y, Urano M, Kenton LA, Kahn J, Willet CG (1991) The accelerated repopulation of a murine fibrosarcoma, FSA-II, during the fractionated irradiation and the linear-quadratic model. Int J Radiat Oncol Biol Phys 21: 1529–1534 - PubMed
-
- Allison P, Franco E, Black M, Feine J (1998) The role of professional diagnostic delays in the prognosis of upper aerodigestive tract carcinoma. Oral Oncol 34: 147–153 - PubMed
-
- Ang KK, Trotti A, Brown BW, Garden AS, Foote RL, Morrison WH, Geara FB, Klotch DW, Goepfert H, Peters LJ (2001) Randomized trial addressing risk features and time factors of surgery plus radiotherapy in advanced head-and-neck cancer. Int J Radiat Oncol Biol Phys 51: 571–578 - PubMed
-
- Awwad HK, Lotayef M, Shouman T, Begg AC, Wilson G, Bentzen SM, Abd El-Moneim H, Eissa S (2002) Accelerated hyperfractionation (AHF) compared to conventional fractionation (CF) in the postoperative radiotherapy of locally advanced head and neck cancer: influence of proliferation. Br J Cancer 86: 517–523 - PMC - PubMed
-
- Balter JM, Ten Haken RK, Lawrence TS, Lam KL, Robertson JM (1996) Uncertainties in CT-based radiation therapy treatment planning associated with patient breathing. Int J Radiat Oncol Biol Phys 36: 167–174 - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

