Laparoscopic versus open appendectomy: outcomes comparison based on a large administrative database
- PMID: 14685099
- PMCID: PMC1356191
- DOI: 10.1097/01.sla.0000103071.35986.c1
Laparoscopic versus open appendectomy: outcomes comparison based on a large administrative database
Abstract
Objective: To compare length of hospital stay, in-hospital complications, in-hospital mortality, and rate of routine discharge between laparoscopic and open appendectomy based on a representative, nationwide database.
Summary background data: Numerous single-institutional randomized clinical trials have assessed the efficacy of laparoscopic and open appendectomy. The results, however, are conflicting, and a consensus concerning the relative advantages of each procedure has not yet been reached.
Methods: Patients with primary ICD-9 procedure codes for laparoscopic and open appendectomy were selected from the 1997 Nationwide Inpatient Sample, a database that approximates 20% of all US community hospital discharges. Multiple linear and logistic regression analyses were used to assess the risk-adjusted endpoints.
Results: Discharge abstracts of 43757 patients were used for our analyses. 7618 patients (17.4%) underwent laparoscopic and 36139 patients (82.6%) open appendectomy. Patients had an average age of 30.7 years and were predominantly white (58.1%) and male (58.6%). After adjusting for other covariates, laparoscopic appendectomy was associated with shorter median hospital stay (laparoscopic appendectomy: 2.06 days, open appendectomy: 2.88 days, P < 0.0001), lower rate of infections (odds ratio [OR] = 0.5 [0.38, 0.66], P < 0.0001), decreased gastrointestinal complications (OR = 0.8 [0.68, 0.96], P = 0.02), lower overall complications (OR = 0.84 [0.75, 0.94], P = 0.002), and higher rate of routine discharge (OR = 3.22 [2.47, 4.46], P < 0.0001).
Conclusions: Laparoscopic appendectomy has significant advantages over open appendectomy with respect to length of hospital stay, rate of routine discharge, and postoperative in-hospital morbidity.
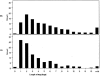
Figures
Comment in
-
Hospital bill in open and laparoscopic appendectomy.Ann Surg. 2004 Sep;240(3):562-3; author reply 563. doi: 10.1097/01.sla.0000138624.33302.44. Ann Surg. 2004. PMID: 15319735 Free PMC article. No abstract available.
References
-
- Samelson SL, Reyes HM. Management of perforated appendicitis in children–revisited. Arch Surg. 1987;122:691–696. - PubMed
-
- Editorial. A sound approach to the diagnosis of acute appendicitis. Lancet. 1987;i:198–200. - PubMed
-
- Semm K. Endoscopic appendectomy. Endoscopy. 1983;15:59–64. - PubMed
-
- Long KH, Bannon MP, Zietlow SP, et al. A prospective randomized comparison of laparoscopic appendectomy with open appendectomy: clinical and economic analyses. Surgery. 2001;129:390–400. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical