Inhibition of alpha-adrenergic vasoconstriction in exercising human thigh muscles
- PMID: 14694145
- PMCID: PMC1664852
- DOI: 10.1113/jphysiol.2003.054650
Inhibition of alpha-adrenergic vasoconstriction in exercising human thigh muscles
Abstract
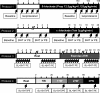
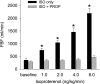
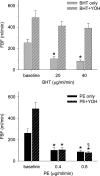
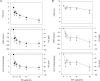
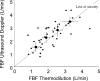
The mechanisms underlying metabolic inhibition of sympathetic responses within exercising skeletal muscle remain incompletely understood. The aim of the present study was to test whether alpha(2)-adrenoreceptor-mediated vasoconstriction was more sensitive to metabolic inhibition than alpha(1)-vasoconstriction during dynamic knee-extensor exercise. We studied healthy volunteers using two protocols: (1) wide dose ranges of the alpha-adrenoreceptor agonists phenylephrine (PE, alpha(1) selective) and BHT-933 (BHT, alpha(2) selective) were administered intra-arterially at rest and during 27 W knee-extensor exercise (n= 13); (2) flow-adjusted doses of PE (0.3 microg kg(-1) l(-1)) and BHT (15 microg kg(-1) l(-1)) were administered at rest and during ramped exercise (7 W to 37 W; n= 10). Ultrasound Doppler and thermodilution techniques provided direct measurements of femoral blood flow (FBF). PE (0.8 microg kg(-1)) and BHT (40 microg kg(-1)) produced comparable maximal reductions in FBF at rest (-58 +/- 6 versus-64 +/- 4%). Despite increasing the doses, PE (1.6 microg kg(-1) min(-1)) and BHT (80 microg kg(-1) min(-1)) caused significantly smaller changes in FBF during 27 W exercise (-13 +/- 4 versus-3 +/- 5%). During ramped exercise, significant vasoconstriction at lower intensities (7 and 17 W) was seen following PE (-16 +/- 5 and -16 +/- 4%), but not BHT (-2 +/- 4 and -4 +/- 5%). At the highest intensity (37 W), FBF was not significantly changed by either drug. Collectively, these data demonstrate metabolic inhibition of alpha-adrenergic vasoconstriction in large postural muscles of healthy humans. Both alpha(1)- and alpha(2)-adrenoreceptor agonists produce comparable vasoconstriction in the resting leg, and dynamic thigh exercise attenuates alpha(1)- and alpha(2)-mediated vasoconstriction similarly. However, alpha(2)-mediated vasoconstriction appears more sensitive to metabolic inhibition, because alpha(2) is completely inhibited even at low workloads, whereas alpha(1) becomes progressively inhibited with increasing workloads.
Figures
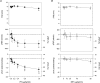
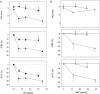
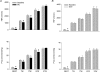
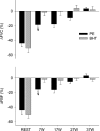
Similar articles
-
Role of {alpha}1-adrenergic vasoconstriction in the regulation of skeletal muscle blood flow with advancing age.Am J Physiol Heart Circ Physiol. 2009 Feb;296(2):H497-504. doi: 10.1152/ajpheart.01016.2008. Epub 2008 Dec 5. Am J Physiol Heart Circ Physiol. 2009. PMID: 19060122 Free PMC article.
-
Exercise-induced inhibition of angiotensin II vasoconstriction in human thigh muscle.J Physiol. 2006 Dec 1;577(Pt 2):727-37. doi: 10.1113/jphysiol.2006.113977. Epub 2006 Sep 14. J Physiol. 2006. PMID: 16973706 Free PMC article.
-
Endothelin-1-mediated vasoconstriction at rest and during dynamic exercise in healthy humans.Am J Physiol Heart Circ Physiol. 2007 Oct;293(4):H2550-6. doi: 10.1152/ajpheart.00867.2007. Epub 2007 Aug 10. Am J Physiol Heart Circ Physiol. 2007. PMID: 17693542
-
Perioperative use of selective alpha-2 agonists and antagonists in small animals.Can Vet J. 2004 Jun;45(6):475-80. Can Vet J. 2004. PMID: 15283516 Free PMC article. Review.
-
Functional sympatholysis in hypertension.Auton Neurosci. 2015 Mar;188:64-8. doi: 10.1016/j.autneu.2014.10.019. Epub 2014 Oct 23. Auton Neurosci. 2015. PMID: 25458424 Free PMC article. Review.
Cited by
-
Role of {alpha}1-adrenergic vasoconstriction in the regulation of skeletal muscle blood flow with advancing age.Am J Physiol Heart Circ Physiol. 2009 Feb;296(2):H497-504. doi: 10.1152/ajpheart.01016.2008. Epub 2008 Dec 5. Am J Physiol Heart Circ Physiol. 2009. PMID: 19060122 Free PMC article.
-
Impaired modulation of postjunctional α1 - but not α2 -adrenergic vasoconstriction in contracting forearm muscle of postmenopausal women.J Physiol. 2018 Jul;596(13):2507-2519. doi: 10.1113/JP275777. Epub 2018 May 30. J Physiol. 2018. PMID: 29708589 Free PMC article. Clinical Trial.
-
Impact of sympathetic nervous system activity on post-exercise flow-mediated dilatation in humans.J Physiol. 2015 Dec 1;593(23):5145-56. doi: 10.1113/JP270946. Epub 2015 Nov 15. J Physiol. 2015. PMID: 26437709 Free PMC article.
-
α-Adrenergic regulation of skeletal muscle blood flow during exercise in patients with heart failure with preserved ejection fraction.J Physiol. 2024 Jul;602(14):3401-3422. doi: 10.1113/JP285526. Epub 2024 Jun 6. J Physiol. 2024. PMID: 38843407 Free PMC article.
-
Taming the "sleeping giant": the role of endothelin-1 in the regulation of skeletal muscle blood flow and arterial blood pressure during exercise.Am J Physiol Heart Circ Physiol. 2013 Jan 1;304(1):H162-9. doi: 10.1152/ajpheart.00603.2012. Epub 2012 Oct 26. Am J Physiol Heart Circ Physiol. 2013. PMID: 23103494 Free PMC article.
References
-
- Andersen P, Adams RP, Sjogaard G, Thorboe A, Saltin B. Dynamic knee extension as model for study of isolated exercising muscle in humans. J Appl Physiol. 1985;59:1647–1653. - PubMed
-
- Anderson KM, Faber JE. Differential sensitivity of arteriolar α1- and α2-adrenoceptor constriction to metabolic inhibition during rat skeletal muscle contraction. Circ Res. 1991;69:174–184. - PubMed
-
- Bangsbo J, Krustrup P, Gonzalez-Alonso J, Boushel R, Saltin B. Muscle oxygen kinetics at onset of intense dynamic exercise in humans. Am J Physiol. 2000;279:R899–R906. - PubMed
-
- Buckwalter JB, Clifford PS. α-Adrenergic vasoconstriction in active skeletal muscles during dynamic exercise. Am J Physiol. 1999;277:H33–H39. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

