Genetic testing among high-risk individuals in families with hereditary nonpolyposis colorectal cancer
- PMID: 14970868
- PMCID: PMC2410159
- DOI: 10.1038/sj.bjc.6601529
Genetic testing among high-risk individuals in families with hereditary nonpolyposis colorectal cancer
Abstract
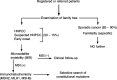
Hereditary nonpolyposis colorectal cancer (HNPCC) is frequently associated with constitutional mutations in a class of genes involved in DNA mismatch repair. We identified 32 kindreds, with germline mutations in one of three genes hMSH2, hMLH1 or hMSH6. In this study, we purposed to evaluate how many high-risk individuals in each family underwent genetic testing: moreover, we assessed how many mutation-positive unaffected individuals accepted colonoscopic surveillance and the main findings of the recommended follow-up. Families were identified through a population-based registry, or referred from other centres. Members of the families were invited for an education session with two members of the staff. When a kindred was consistent with HNPCC, neoplastic tissues were examined for microsatellite instability (MSI) and immunohistochemical expression of MSH2, MLH1 and MSH6 proteins. Moreover, constitutional mutations were searched by SSCP or direct sequencing of the whole genomic region. Of the 164 subjects assessed by genetic testing, 89 were gene carriers (66 affected - that is, with HNPCC-related cancer diagnosis - and 23 unaffected) and 75 tested negative. Among the 23 unaffected gene carriers, 18 (78.3%) underwent colonoscopy and four declined. On a total of 292 first degree at risk of cancer, 194 (66.4%) did not undergo genetic testing. The main reasons for this were: (a) difficulty to reach family members at risk, (b) lack of collaboration, (c) lack of interest in preventive medicine or 'fatalistic' attitude towards cancer occurrence. The number of colorectal lesions detected at endoscopy in gene carriers was significantly (P<0.01) higher than in controls (noncarriers). We conclude that a large fraction of high-risk individuals in mutation-positive HNPCC families does not undergo genetic testing, despite the benefits of molecular screening and endoscopic surveillance. This clearly indicates that there are still barriers to genetic testing in HNPCC, and that we are unable to provide adequate protection against cancer development in these families.
Figures
References
-
- Aaltonen LA, Peltomaki P, Leach FS, Sistonen P, Pylkkanen L, Mecklin JP, Jarvinen H, Powell SM, Jen J, Hamilton SR, Petersen GM, Kinzler KW, Vogelstein B, de la Chapelle A (1993) Clues to the pathogenesis of familial colorectal cancer. Science 260: 812–816 - PubMed
-
- Aaltonen LA, Salovaara R, Kristo P, Canzian F, Hemminki A, Peltomaki P, Chadwick RB, Kaariainen H, Eskelinen M, Jarvinen H, Mecklin JP, de la Chapelle A (1998) Incidence of hereditary nonpolyposis colorectal cancer and the feasibility of molecular screening for the disease. N Engl J Med 338: 1481–1487 - PubMed
-
- Black RJ, Bray F, Ferlay JM, Parkin DM (1997) Cancer incidence and mortality in the European Union: cancer registry data and estimates of national incidence for 1990. Eur J Cancer 33: 1075–1107 - PubMed
-
- Calvert PM, Frucht H (2002) The genetics of colorectal cancer. Ann Intern Med 137: 603–612 - PubMed
-
- de Vos tot Nederveen Cappel WH, Nagengast FM, Griffioen G, Menko FH, Taal BG, Kleibeuker JH, Vasen HF (2002) Surveillance for hereditary nonpolyposis colorectal cancer. A long-term study on 114 families. Dis Colon Rectum 45: 1588–1594 - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

