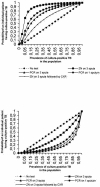
Comparison of PCR with the routine procedure for diagnosis of tuberculosis in a population with high prevalences of tuberculosis and human immunodeficiency virus
- PMID: 15004046
- PMCID: PMC356878
- DOI: 10.1128/JCM.42.3.1012-1015.2004
Comparison of PCR with the routine procedure for diagnosis of tuberculosis in a population with high prevalences of tuberculosis and human immunodeficiency virus
Abstract
Direct smear examination with Ziehl-Neelsen (ZN) staining for the diagnosis of tuberculosis (TB) as employed in most low-income countries is cheap and easy to use, but its low sensitivity is a major drawback. The low specificity of chest X-rays, used for the diagnosis of smear-negative TB, risks high levels of overdiagnosis. Major advances in molecular techniques, which rapidly identify mycobacterial DNA in sputa, may overcome these obstacles. In this study, the AMPLICOR PCR system was used to diagnose pulmonary TB in a developing country with high prevalences of both TB and human immunodeficiency virus (HIV). The sensitivity and specificity of this technique were compared to those of the usual diagnostic techniques. Sputum specimens were collected from 1,396 TB suspects attending the Rhodes Chest Clinic, Nairobi, Kenya. The specimens were analyzed for the presence of Mycobacterium tuberculosis by PCR; culture on Löwenstein-Jensen medium was used as the "gold standard." All culture-positive samples were genotyped to identify the mycobacterial species. The sensitivity and specificity of PCR were 93 and 84%, respectively. HIV status did not affect the sensitivity of PCR. A total of 99.7% of the true smear-positive and 82.1% of the true smear-negative TB patients were correctly identified by PCR. PCR detected M. tuberculosis in 11.7% of the culture-negative suspects, 60% of which had one or two PCR-positive sputum specimens. Of the 490 positive cultures, 486 were identified as M. tuberculosis. The high sensitivity of Amplicor PCR merits usage in a clinical setting with high TB and HIV burdens. Thus, PCR can be considered as an alternative to ZN staining in combination with chest X-ray for diagnosis of TB; however, cost-effectiveness studies and operational studies are required to support an evidence-based decision of introducing PCR for TB control in high-burden environments.
Figures
References
-
- Böttger, E. C. 1996. Approaches for identification of microorganisms. ASM News 62:247-250.
-
- Daar, A. S., H. Thorsteinsdottir, D. K. Martin, A. C. Smith, S. Nast, and P. A. Singer. 2002. Top ten biotechnologies for improving health in developing countries. Nat. Genet. 32:229-232. - PubMed
-
- Kambashi, B., G. Mbulo, R. McNerney, R. Tembwe, A. Kambashi, V. Tihon, and P. Godfrey-Faussett. 2001. Utility of nucleic acid amplification techniques for the diagnosis of pulmonary tuberculosis in sub-Saharan Africa. Int. J. Tuberc. Lung Dis. 5:364-369. - PubMed
-
- Kaul, K. L. 2001. Molecular detection of Mycobacterium tuberculosis: impact on patient care. Clin. Chem. 47:1553-1558. - PubMed
-
- Kent, P. T., and G. P. Kubica. 1985. Public health laboratory. A guide for the level III laboratory. U.S. Department of Health and Human Services publication no. (CDC) 86-8230. Centers for Disease Control and Prevention, Atlanta, Ga.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical