Relationship between circle of Willis morphology on 3D time-of-flight MR angiograms and transient ischemia during vascular clamping of the internal carotid artery during carotid endarterectomy
- PMID: 15090341
- PMCID: PMC7975596
Relationship between circle of Willis morphology on 3D time-of-flight MR angiograms and transient ischemia during vascular clamping of the internal carotid artery during carotid endarterectomy
Abstract
Background and purpose: A potential source of complication at carotid endarterectomy (CEA) is cerebral ischemia caused by hypoperfusion during clamping of the carotid artery. Configuration of primary collateral pathways may be a major risk factor for development of transient cerebral ischemia during clamping. We investigated whether circle of Willis morphology on 3D time-of-flight (TOF) MR angiograms can reliably predict transient ischemia during vascular clamping of the internal carotid artery (ICA) in patients undergoing CEA.
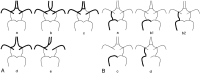
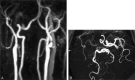
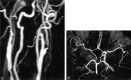
Methods: Three-dimensional TOF MR angiography and CEA were performed in 117 patients. Patients had unilateral stenosis (n = 86), unilateral stenosis with contralateral occlusion (n = 21), or bilateral severe stenosis (n = 10) of the ICA. Circle of Willis morphology on preoperative 3D TOF MR angiograms was analyzed and correlated with intraoperative history of ischemia during vascular clamping of the ICA.
Results: Patients with unilateral stenosis or bilateral severe stenosis experienced transient ischemia during clamping of ICA at a low rate (11 [11%] of 96). In these groups, we found no specific circle of Willis patterns associated with development of intraoperative ischemia. However, patients with contralateral ICA occlusion experienced ischemia frequently during clamping of the ICA (12 [57%] of 21). In this group, incompleteness of the circle of Willis was significantly related to the risk of intraoperative ischemia (P =.005).
Conclusion: In patients without contralateral ICA occlusion, circle of Willis morphology on 3D TOF MR angiograms cannot predict the development of intraoperative ischemia. However, in patients with contralateral ICA occlusion, incompleteness of the posterior part of the circle of Willis is a significant risk factor for development of ischemia during vascular clamping of the ICA.
Figures
References
-
- Rutgers DR, Blankensteijn JD, Van der Grond J. Preoperative MRA flow quantification in CEA patients: flow differences between patients who develop cerebral ischemia and patients who do not develop cerebral ischemia during cross-clamping of the carotid artery. Stroke 2000;31:3021–3028 - PubMed
-
- North American Symptomatic Carotid Endarterectomy Trial Collaborators. Beneficial effect of carotid endarterectomy in symptomatic patients with high-grade carotid stenosis. N Engl J Med 1991;325:445–453 - PubMed
-
- Depippo PS, Ascher E, Scheinman M, Yorkovich W, Hingorani A. The value and limitations of magnetic resonance angiography of the circle of Willis in patients undergoing carotid endarterectomy. Cardiovasc Surg 1999;7:27–32 - PubMed
-
- Lopez-Bresnahan MV, Kearse LA Jr, Yanez P, Young TI. Anterior communicating artery collateral flow protection against ischemic change during carotid endarterectomy. J Neurosurg 1993;79:379–382 - PubMed
-
- Zampella E, Morawetz RB, McDowell HA, et al. The importance of cerebral ischemia during carotid endarterectomy. Neurosurgery 1991;29:727–731 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
