Myocardial perfusion scintigraphy: the evidence
- PMID: 15129710
- PMCID: PMC2562441
- DOI: 10.1007/s00259-003-1344-5
Myocardial perfusion scintigraphy: the evidence
Abstract
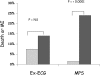
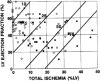
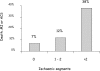
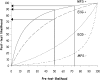
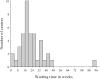
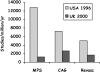
This review summarises the evidence for the role of myocardial perfusion scintigraphy (MPS) in patients with known or suspected coronary artery disease. It is the product of a consensus conference organised by the British Cardiac Society, the British Nuclear Cardiology Society and the British Nuclear Medicine Society and is endorsed by the Royal College of Physicians of London and the Royal College of Radiologists. It was used to inform the UK National Institute of Clinical Excellence in their appraisal of MPS in patients with chest pain and myocardial infarction. MPS is a well-established, non-invasive imaging technique with a large body of evidence to support its effectiveness in the diagnosis and management of angina and myocardial infarction. It is more accurate than the exercise ECG in detecting myocardial ischaemia and it is the single most powerful technique for predicting future coronary events. The high diagnostic accuracy of MPS allows reliable risk stratification and guides the selection of patients for further interventions, such as revascularisation. This in turn allows more appropriate utilisation of resources, with the potential for both improved clinical outcomes and greater cost-effectiveness. Evidence from modelling and observational studies supports the enhanced cost-effectiveness associated with MPS use. In patients presenting with stable or acute chest pain, strategies of investigation involving MPS are more cost-effective than those not using the technique. MPS also has particular advantages over alternative techniques in the management of a number of patient subgroups, including women, the elderly and those with diabetes, and its use will have a favourable impact on cost-effectiveness in these groups. MPS is already an integral part of many clinical guidelines for the investigation and management of angina and myocardial infarction. However, the technique is underutilised in the UK, as judged by the inappropriately long waiting times and by comparison with the numbers of revascularisations and coronary angiograms performed. Furthermore, MPS activity levels in this country fall far short of those in comparable European countries, with about half as many scans being undertaken per year. Currently, the number of MPS studies performed annually in the UK is 1,200/million population/year. We estimate the real need to be 4,000/million/year. The current average waiting time is 20 weeks and we recommend that clinically appropriate upper limits of waiting time are 6 weeks for routine studies and 1 week for urgent studies.
Figures



References
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'DOI', 'value': '10.1001/jama.217.8.1061', 'is_inner': False, 'url': 'https://doi.org/10.1001/jama.217.8.1061'}, {'type': 'PubMed', 'value': '5109427', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/5109427/'}]}
- Rochmis P, Blackburn H. Exercise tests. A survey of procedures, safety and litigation experience in approximately 170,000 tests. JAMA 1971; 217:1061–1066. - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '8294691', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/8294691/'}]}
- Cerqueira MD, Verani MS, Schwaiger M, et al. Safety profile of adenosine stress perfusion imaging: results from the Adenoscan multicenter trial registry. J Am Coll Cardiol 1994; 23:3849. - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '9420757', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/9420757/'}]}
- Lette J, Tatum JL, Fraser S, et al. Safety of dipyridamole testing in 73,806 patients: the multicentre dipyridamole safety study. J Nucl Cardiol 1995; 2:3–17. - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '8319327', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/8319327/'}]}
- Mertes H, Sawada SG, Ryan T, et al. Symptoms, adverse effects, and complications associated with dobutamine stress echocardiography: experience in 1118 patients. Circulation 1993; 88:15–19. - PubMed
-
- Administration of Radioactive Substances Advisory Committee. Notes for guidance on the clinical administration of radiopharmaceuticals and use of sealed radioactive sources. Didcot, UK: ARSAC Support Unit, National Radiological Protection Board, 1998.

