Specific binding to intracellular proteins determines arterial transport properties for rapamycin and paclitaxel
- PMID: 15197278
- PMCID: PMC438999
- DOI: 10.1073/pnas.0400918101
Specific binding to intracellular proteins determines arterial transport properties for rapamycin and paclitaxel
Abstract
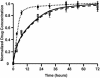
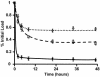
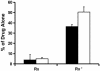
Endovascular drug-eluting stents have changed the practice of medicine, and yet it is unclear how they so dramatically reduce restenosis and how to distinguish between the different formulations available. Biological drug potency is not the sole determinant of biological effect. Physicochemical drug properties also play important roles. Historically, two classes of therapeutic compounds emerged: hydrophobic drugs, which are retained within tissue and have dramatic effects, and hydrophilic drugs, which are rapidly cleared and ineffective. Researchers are now questioning whether individual properties of different drugs beyond lipid avidity can further distinguish arterial transport and distribution. In bovine internal carotid segments, tissue-loading profiles for hydrophobic paclitaxel and rapamycin are indistinguishable, reaching load steady state after 2 days. Hydrophilic dextran reaches equilibrium in several hours at levels no higher than surrounding solution concentrations. Both paclitaxel and rapamycin bind to the artery at 30-40 times bulk concentration. Competitive binding assays confirm binding to specific tissue elements. Most importantly, transmural drug distribution profiles are markedly different for the two compounds, reflecting, perhaps, different modes of binding. Rapamycin, which binds specifically to FKBP12 binding protein, distributes evenly through the artery, whereas paclitaxel, which binds specifically to microtubules, remains primarily in the subintimal space. The data demonstrate that binding of rapamycin and paclitaxel to specific intracellular proteins plays an essential role in determining arterial transport and distribution and in distinguishing one compound from another. These results offer further insight into the mechanism of local drug delivery and the specific use of existing drug-eluting stent formulations.
Figures
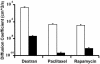

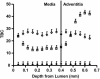
References
-
- Hwang, C. W., Wu, D. & Edelman, E. R. (2001) J. Am. Coll. Cardiol. 37, Suppl. A, 1A-2A. - PubMed
-
- Hwang, C. W., Wu, D. & Edelman, E. R. (2001) Circulation 104, 600-605. - PubMed
-
- Hwang, C. W. & Edelman, E. R. (2002) Circ. Res. 90, 826-832. - PubMed
-
- Lovich, M. A., Brown, L. & Edelman, E. R. (1997) J. Am. Coll. Cardiol. 29, 1645-1650. - PubMed
-
- Lovich, M. A. & Edelman, E. R. (1995) Circ. Res. 77, 1143-1150. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

