Forty consecutive resections of hilar cholangiocarcinoma with no postoperative mortality and no positive ductal margins: results of a prospective study
- PMID: 15213624
- PMCID: PMC1356380
- DOI: 10.1097/01.sla.0000129491.43855.6b
Forty consecutive resections of hilar cholangiocarcinoma with no postoperative mortality and no positive ductal margins: results of a prospective study
Abstract
Objective: Our objective was to perform a prospective study of surgical treatment of hilar cholangiocarcinoma according to newly established guidelines for performing safe and curative resections.
Summary background data: The poor survival rate after resection of hilar cholangiocarcinoma is considered to be mainly the result of in-hospital death and positive ductal margins.
Methods: Between July 1999 and December 2002, 40 of 42 surgically explored patients with hilar cholangiocarcinoma underwent resection. They were managed with preoperative biliary decompression, portal embolization, cholangiographic evaluation, and a choice of surgical procedures and techniques.
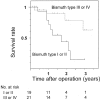
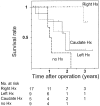
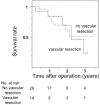
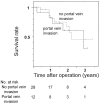
Results: Hospital or 30-day mortality and morbidity rates were 0% and 48%, respectively. Hepatic failure was not encountered. Histopathologic examination revealed no positive ductal margins in all 40 patients, but 2 showed positive separation margins from the right hepatic artery. The overall 3-year survival rate and median survival time were 40% and 27 months. Survival of patients with Bismuth type III or IV tumors or of patients who underwent right hepatectomy was significantly better. Survival of patients who underwent concomitant vascular resection was similar to survival of those who did not. Univariate analysis indicated the type of hepatectomy, histopathologic grade, Bismuth classification, concomitant hepatic artery resection, and International Union Against Cancer stage as significant prognostic factors.
Conclusions: No postoperative mortality and no positive ductal margins were achieved according to the above guidelines in a high-volume expert center. Long-term results, however, have not been significantly improved. A survival analysis of the patient series with homogeneous conditions derived from a short study period suggests the need for additional strategies including right hepatectomy for Bismuth type I or II tumors.
Figures
References
-
- Nimura Y, Hayakawa N, Kamiya J, et al. Hepatic segmentectomy with caudate lobe resection for bile duct carcinoma of the hepatic hilus. World J Surg. 1990;4:533–544. - PubMed
-
- Saldinger PF, Blumgart LH. Resection of hilar cholangiocarcinoma: a European and United States experience. J Hepatobiliary Pancreat Surg. 2000;7:111–114. - PubMed
-
- Klempnauer J, Ridder GJ, von Wasielewski R, et al. Resectional surgery of hilar cholangiocarcinoma: a multivariate analysis of prognostic factors. J Clin Oncol. 1997;15:947–954. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

