Incidence of cerebral metastases in patients treated with trastuzumab for metastatic breast cancer
- PMID: 15266327
- PMCID: PMC2364775
- DOI: 10.1038/sj.bjc.6601970
Incidence of cerebral metastases in patients treated with trastuzumab for metastatic breast cancer
Abstract
Trastuzumab is an effective treatment for patients with metastatic breast cancer (MBC) that overexpresses HER-2. A high incidence of brain metastases (BM) has been noted in patients receiving trastuzumab. A retrospective chart review was conducted of 100 patients commencing trastuzumab for metastatic breast cancer from July 1999 to December 2002, at the Christie Hospital. Seven patients were excluded; five patients developed central nervous system metastases prior to starting trastuzumab, and inadequate data were available for two. Out of the remaining 93 patients, 23 (25%) have developed BM to date. In all, 46 patients have died, and of these 18 (39%) have been diagnosed with BM prior to death. Of the 23 patients developing BM, 18 (78%) were hormone receptor negative and 18 (78%) had visceral disease. Univariate analysis showed a significant association between the development of cerebral disease and both hormone receptor status and the presence of visceral disease. In conclusion, a high proportion of patients with MBC treated with trastuzumab develop symptomatic cerebral metastases. HER-2-positive breast cancer may have a predilection for the brain, or trastuzumab therapy may change the disease pattern by prolonging survival. New strategies to address this problem require investigation in this group of patients.
Figures

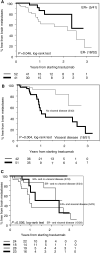
References
-
- Baculi RH, Suki S, Nisbett J, Leeds N, Groves M (2001) Meningeal carcinomatosis from breast carcinoma responsive to trastuzumab. J Clin Oncol 19: 3297–3298 - PubMed
-
- Bendell JC, Domchek SM, Burnstein HJ, Harris L, Younger J, Kuter I, Bunnell C, Rue M, Gelman R, Winer E (2003) Central nervous system metastases in women who receive trastuzumab-based therapy for metastatic breast carcinoma. Cancer 97: 2972–2977 - PubMed
-
- Brufsky AM, Cleary D, Fuchs C, Lebish J, Baar J, Evans T, Lembersky B, Belani CP (2003) First-line chemotherapy for metastatic breast cancer (MBC) with docetaxel (T), carboplatin (C), and trastuzumab (H) (TCH): a phase II trial. Proc Am Soc Clin Oncol 22: A71
-
- Clark GM, Sledge Jr GW, Osborne CK, McGuire WL (1987) Survival from first recurrence: relative importance of prognostic factors in 1015 breast cancer patients. J Clin Oncol 5: 55–61 - PubMed
-
- Cobleigh MA, Vogel CL, Tripathy D, Robert NJ, Scholl S, Frenbacher L, Wolter JM, Paton V, Shak S, Lieberman G, Slamon DJ (1999) Multinational study of the efficacy and safety of humanised anti-HER2 monoclonal antibody in women who have HER2-overexpressing metastatic breast cancer that has progressed after chemotherapy for metastatic disease. J Clin Oncol 17: 2639–2648 - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

