A primary amelanotic melanoma of the vagina, diagnosed by immunohistochemical staining with HMB-45, which recurred as a pigmented melanoma
- PMID: 15333663
- PMCID: PMC1770413
- DOI: 10.1136/jcp.2004.016220
A primary amelanotic melanoma of the vagina, diagnosed by immunohistochemical staining with HMB-45, which recurred as a pigmented melanoma
Abstract
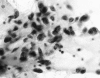
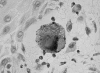
Usually, malignant melanoma is readily diagnosed by the presence of melanin granules. Although amelanotic melanoma contains a few melanin granules, it is often difficult to differentiate from non-epithelial malignant tumours. This report describes a case of amelanotic melanoma of the vagina, which was originally suspected to be a non-epithelial malignant tumour, but was subsequently correctly diagnosed by immunohistochemical staining with the HMB-45 antibody and for the S-100 protein. A light grey tumour with superficial ulceration was located in the upper third of the vagina. The patient was treated with irradiation followed by chemotherapy. Subsequently, the tumour disappeared and cytology was negative; thus, she achieved complete remission. However, 20 months after complete remission, the tumour recurred locally: the site had a grossly black appearance, which was pathognomonic for a malignant melanoma. Thus, HMB-45 and S-100 protein immunohistochemistry confirmed the diagnosis of amelanotic melanoma.
Figures

Similar articles
-
Amelanotic vulvar melanoma: case report and review of the literature.Rom J Morphol Embryol. 2008;49(2):219-28. Rom J Morphol Embryol. 2008. PMID: 18516330 Review.
-
Primary amelanotic melanoma of the vagina.Onkologie. 2008 Sep;31(8-9):474-6. doi: 10.1159/000142398. Epub 2008 Aug 12. Onkologie. 2008. PMID: 18787356
-
[Clinical analysis of 42 cases of primary malignant melanoma in female genital tract].Zhonghua Fu Chan Ke Za Zhi. 2007 May;42(5):320-4. Zhonghua Fu Chan Ke Za Zhi. 2007. PMID: 17673044 Chinese.
-
Amelanotic vulvar melanoma with intratumor histological heterogeneity.J Dermatol. 2010 Jun;37(6):537-41. doi: 10.1111/j.1346-8138.2010.00895.x. J Dermatol. 2010. PMID: 20536668
-
Primary malignant vaginal melanoma treated with adriamycin and ifosfamide: a case report and literature review.Gynecol Oncol. 2005 May;97(2):700-3. doi: 10.1016/j.ygyno.2005.02.013. Gynecol Oncol. 2005. PMID: 15863186 Review.
Cited by
-
Nevoid melanoma of the vagina: report of one case diagnosed on thin layer cytological preparations.Cytojournal. 2007 Jul 3;4:14. doi: 10.1186/1742-6413-4-14. Cytojournal. 2007. PMID: 17608945 Free PMC article.
-
Malignant melanoma of the vagina: A case report and review of the literature.Oncol Lett. 2014 Oct;8(4):1585-1588. doi: 10.3892/ol.2014.2357. Epub 2014 Jul 17. Oncol Lett. 2014. PMID: 25202372 Free PMC article.
-
Amelanotic melanoma masquerading as a superficial small round cell tumor: a diagnostic challenge.Indian J Dermatol. 2014 Nov;59(6):631. doi: 10.4103/0019-5154.143569. Indian J Dermatol. 2014. PMID: 25484414 Free PMC article.
-
Metastatic malignant melanoma of the small bowel--report of two cases.J Gastrointest Cancer. 2012 Jun;43(2):332-5. doi: 10.1007/s12029-010-9180-x. J Gastrointest Cancer. 2012. PMID: 20607448
-
Primary Anorectal Amelanotic Melanoma: The First Case Report from Saudi Arabia.Middle East J Dig Dis. 2019 Jul;11(3):166-173. doi: 10.15171/mejdd.2019.144. Epub 2019 May 22. Middle East J Dig Dis. 2019. PMID: 31687116 Free PMC article.
References
-
- Creasman WT, Phillips JL, Menck HR. The National Cancer Data Base report on cancer of the vagina. Cancer 1998;83:1033–40. - PubMed
-
- Perniciaro C. Dermatopathologic variants of malignant melanoma. Mayo Clin Proc 1997;72:273–9. - PubMed
-
- Giuliano AE, Cochran AJ, Morton DL. Melanoma from unknown primary site and amelanotic melanoma. Semin Oncol 1982;9:442–7. - PubMed
-
- Scambia G, Benedetti Panici P, Baiocchi G, et al. A primary amelanotic melanoma of the vagina diagnosed by immunocytochemistry. Int J Gynaecol Obstet 1989;29:159–64. - PubMed
-
- Ragnarsson-Olding B, Johansson H, Rutqvist LE, et al. Malignant melanoma of the vulva and vagina. Trends in incidence, age distribution, and long-term survival among 245 consecutive cases in Sweden 1960–1984. Cancer 1993;71:1893–7. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
