Epidemiology and clinical features of bloodstream infections caused by AmpC-type-beta-lactamase-producing Klebsiella pneumoniae
- PMID: 15388426
- PMCID: PMC521917
- DOI: 10.1128/AAC.48.10.3720-3728.2004
Epidemiology and clinical features of bloodstream infections caused by AmpC-type-beta-lactamase-producing Klebsiella pneumoniae
Abstract
Cases of bacteremia caused by AmpC-type-beta-lactamase-producing Klebsiella pneumoniae isolates were retrospectively studied to determine the epidemiologic features and clinical outcomes of bloodstream infections. Among 389 blood isolates recovered from 1998 to 2002, 65 isolates (16.7%) were found to be extended-spectrum beta-lactamase (ESBL) or AmpC beta-lactamase producers. The beta-lactamases from 61 of the 65 isolates were characterized; 28 of 61 isolates produced AmpC-type enzymes (14 isolates each produced DHA-1 and CMY-1-like enzymes), 32 isolates produced TEM or SHV-related ESBLs, and 1 isolate produced a CTX-M-14-like enzyme. To compare the clinical features and outcomes of bloodstream infections caused by AmpC producers with those caused by TEM- or SHV-related ESBL producers, 27 patients infected with isolates producing AmpC-type enzymes (AmpC group) and 25 patients infected with isolates producing TEM- or SHV-related enzymes (ESBL group) were analyzed. There was no significant difference between the AmpC and the ESBL groups in terms of risk factors. When the initial response was assessed at 72 h after antimicrobial therapy, the treatment failure rate for the AmpC group was 51.9% (14 of 27 patients) and the 7- and 30-day mortality rates were 14.8 and 29.6%, respectively, which were similar to those for the ESBL group. When the mortality rate for the patients who received extended-spectrum cephalosporins as definitive treatment was assessed, all four patients in the DHA-1 group and one of three patients in the CMY-1-like group died. In summary, the prevalence of AmpC enzyme-producing K. pneumoniae was high at the Seoul National University Hospital, and the clinical features and outcomes for the patients infected with AmpC-producing organisms were similar to those for the patients infected with TEM- or SHV-related ESBL producers.
Figures


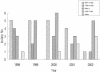
References
-
- Bauernfeind, A., Y. Chong, and S. Schweighart. 1989. Extended broad spectrum β-lactamase in Klebsiella pneumoniae including resistance to cephamycins. Infection 17:316-321. - PubMed
-
- Bradford, P. A., C. Urban, N. Mariano, S. J. Projan, J. J. Rahal, and K. Bush. 1997. Imipenem resistance in Klebsiella pneumoniae is associated with the combination of ACT-1, a plasmid-mediated AmpC β-lactamase, and the loss of an outer membrane protein. Antimicrob. Agents Chemother. 41:563-569. - PMC - PubMed
-
- Garner, J. S., W. R. Jarvis, T. G. Emori, T. C. Horan, and J. M. Hughes. 1988. CDC definitions for nosocomial infections. Am. J. Infect. Control 16:128-140. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

