Pylorus preserving pancreaticoduodenectomy versus standard Whipple procedure: a prospective, randomized, multicenter analysis of 170 patients with pancreatic and periampullary tumors
- PMID: 15492552
- PMCID: PMC1356476
- DOI: 10.1097/01.sla.0000143248.71964.29
Pylorus preserving pancreaticoduodenectomy versus standard Whipple procedure: a prospective, randomized, multicenter analysis of 170 patients with pancreatic and periampullary tumors
Abstract
Objective: A prospective randomized multicenter study was performed to assess whether the results of pylorus-preserving pancreaticoduodenectomy (PPPD) equal those of the standard Whipple (SW) operation, especially with respect to duration of surgery, blood loss, hospital stay, delayed gastric emptying (DGE), and survival.
Summary background data: PPPD has been associated with a higher incidence of delayed gastric emptying, resulting in a prolonged period of postoperative nasogastric suctioning. Another criticism of the pylorus-preserving pancreaticoduodenectomy for patients with a malignancy is the radicalness of the resection. On the other hand, PPPD might be associated with a shorter operation time and less blood loss.
Methods: A prospective randomized multicenter study was performed in a nonselected series of 170 consecutive patients. All patients with suspicion of pancreatic or periampullary tumor were included and randomized for a SW or a PPPD resection. Data concerning patients' demographics, intraoperative and histologic findings, as well as postoperative mortality, morbidity, and follow-up up to 115 months after discharge, were analyzed.
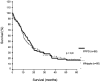
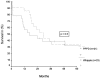
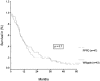
Results: There were no significant differences noted in age, sex distribution, tumor localization, and staging. There were no differences in median blood loss and duration of operation between the 2 techniques. DGE was observed equally in the 2 groups. There was only a marginal difference in postoperative weight loss in favor of the standard Whipple procedure. Overall operative mortality was 5.3%. Tumor positive resection margins were found for 12 patients of the SW group and 19 patients of the PPPD group (P < 0.23). Long-term follow-up showed no significant statistical differences in survival between the 2 groups (P < 0.90).
Conclusions: The SW and PPPD operations were associated with comparable operation time, blood loss, hospital stay, mortality, morbidity, and incidence of DGE. The overall long-term and disease-free survival was comparable in both groups. Both surgical procedures are equally effective for the treatment of pancreatic and periampullary carcinoma.
Figures
Comment in
-
Save the pylori.Ann Surg. 2004 Nov;240(5):746-7. doi: 10.1097/01.sla.0000144690.54204.d3. Ann Surg. 2004. PMID: 15492553 Free PMC article. No abstract available.
References
-
- Cooperman AM. Pancreatic cancer: the bigger picture. Surg Clin North Am. 2001;81:557–574. - PubMed
-
- Mosca F, Giulianotti PC, Balestracci T, et al. Long-term survival in pancreatic cancer: pylorus-preserving versus Whipple pancreatoduodenectomy. Surgery. 1997;122:553–566. - PubMed
-
- Richter A, Niedergethmann M, Sturm JW, et al. Long-term results of partial pancreaticoduodenectomy for ductal adenocarcinoma of the pancreatic head: 25-year experience. World J Surg. 2003;27:324–329. - PubMed
-
- Trede M, Saeger HD, Schwall G, et al. Resection of pancreatic cancer: surgical achievements. Langenbecks Arch Surg. 1998;383:121–128. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical