Optical properties of human prostate at 732 nm measured in mediated photodynamic therapy
- PMID: 15535736
- PMCID: PMC4474534
- DOI: 10.1562/2004-06-25-RA-216
Optical properties of human prostate at 732 nm measured in mediated photodynamic therapy
Abstract
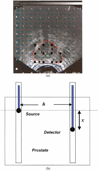
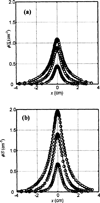
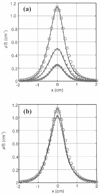
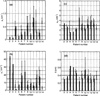
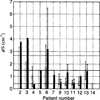
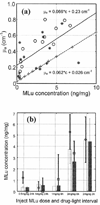
Characterization of the tissue light penetration in prostate photodynamic therapy (PDT) is important to plan the arrangement and weighting of light sources so that sufficient light fluence is delivered to the treatment volume. The optical properties (absorption [mu(a)], transport scattering [mu(s)'] and effective attenuation [mu(eff)] coefficients) of 13 patients with locally recurrent prostate cancer were measured in situ using interstitial isotropic detectors. Measurements were made at 732 nm before and after motexafin lutetium (MLu)-mediated PDT in four quadrants. Optical properties were derived by applying the diffusion theory to the fluence rates measured at several distances (0.5-5 cm) from a point source. mu(a) and mu(s)' varied between 0.07 and 1.62 cm(-1) (mean 0.37 +/- 0.24 cm(-1)) and 1.1 and 44 cm(-1) (mean 14 +/- 11 cm(-1)), respectively. mu(a) was proportional to the concentration of MLu measured by an ex vivo fluorescence assay. We have observed, on average, a reduction of the MLu concentration after PDT, presumably due to the PDT consumption of MLu. mu(eff) varied between 0.91 and 6.7 cm(-1) (mean 2.9 +/- 0.7 cm(-1)), corresponding to an optical penetration depth (delta = 1/micro(eff)) of 0.1-1.1 cm (mean 0.4 +/- 0.1 cm). The mean penetration depth at 732 nm in human prostate is at least two times smaller than that found in normal canine prostates, which can be explained by a four times increase of the mean value of mu(s)' in human prostates. The mean light fluence rate per unit source strength at 0.5 cm from a point source was 1.5 +/- 1.1 cm(-2), excluding situations when bleeding occurs. The total number of measurements was N = 121 for all mean quantities listed above. This study showed significant inter- and intraprostatic differences in the optical properties, suggesting that a real-time dosimetry measurement and feedback system for monitoring light fluences during treatment should be considered for future PDT studies.
Figures

References
-
- Hsi RA, Rosenthal DI, Glatstein E. Photodynamic therapy in the treatment of cancer: current state of the art. Drugs. 1999;57:725–734. - PubMed
-
- D’Amico AV. Role of interstitial radiotherapy in the management of clinically organ-confined prostate cancer: the jury is still out. J. Clin. Oncol. 1996;14:304–315. - PubMed
-
- Chang SC, Buonaccorsi G, MacRobert A, Bown SG. Interstitial photodynamic therapy of the canine prostate using meso-tetra-(m-hydroxyphenyl) chlorine. Int. J. Cancer. 1996;67:555–562. - PubMed
-
- Selman SH, Keck RW, Hampton JA. Transperineal photodynamic ablation of the canine prostate. J. Urol. 1996;156:258–260. - PubMed
-
- Chang SC, Buonaccorsi G, MacRobert A, Bown SG. Interstitial photodynamic therapy of the canine prostate with disulfo-nated aluminum phthalocyanine and 5-aminolevulinic acid-induced protoporphyrin IX. Prostate. 1997;32:89–98. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

