Adoptive immunotherapy of cancer with polyclonal, 108-fold hyperexpanded, CD4+ and CD8+ T cells
- PMID: 15566571
- PMCID: PMC535812
- DOI: 10.1186/1479-5876-2-41
Adoptive immunotherapy of cancer with polyclonal, 108-fold hyperexpanded, CD4+ and CD8+ T cells
Abstract
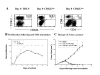
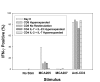
T cell-mediated cancer immunotherapy is dose dependent and optimally requires participation of antigen-specific CD4+ and CD8+ T cells. Here, we isolated tumor-sensitized T cells and activated them in vitro using conditions that led to greater than 108-fold numerical hyperexpansion of either the CD4+ or CD8+ subset while retaining their capacity for in vivo therapeutic efficacy. Murine tumor-draining lymph node (TDLN) cells were segregated to purify the CD62Llow subset, or the CD4+ subset thereof. Cells were then propagated through multiple cycles of anti-CD3 activation with IL-2 + IL-7 for the CD8+ subset, or IL-7 + IL-23 for the CD4+ subset. A broad repertoire of TCR Vbeta families was maintained throughout hyperexpansion, which was similar to the starting population. Adoptive transfer of hyper-expanded CD8+ T cells eliminated established pulmonary metastases, in an immunologically specific fashion without the requirement for adjunct IL-2. Hyper-expanded CD4+ T cells cured established tumors in intracranial or subcutaneous sites that were not susceptible to CD8+ T cells alone. Because accessibility and antigen presentation within metastases varies according to anatomic site, maintenance of a broad repertoire of both CD4+ and CD8+ T effector cells will augment the overall systemic efficacy of adoptive immunotherapy.
Figures



Similar articles
-
Adoptive immunotherapy of advanced tumors with CD62 L-selectin(low) tumor-sensitized T lymphocytes following ex vivo hyperexpansion.J Immunol. 2002 Sep 15;169(6):3314-20. doi: 10.4049/jimmunol.169.6.3314. J Immunol. 2002. PMID: 12218152
-
Different cytokine profiles released by CD4+ and CD8+ tumor-draining lymph node cells involved in mediating tumor regression.J Leukoc Biol. 1997 Apr;61(4):507-16. doi: 10.1002/jlb.61.4.507. J Leukoc Biol. 1997. PMID: 9103238
-
Cellular interactions in effector cell generation and tumor regression mediated by anti-CD3/interleukin 2-activated tumor-draining lymph node cells.Cancer Res. 1992 Mar 1;52(5):1129-36. Cancer Res. 1992. PMID: 1531321
-
Helper-independent, L-selectinlow CD8+ T cells with broad anti-tumor efficacy are naturally sensitized during tumor progression.J Immunol. 2000 Nov 15;165(10):5738-49. doi: 10.4049/jimmunol.165.10.5738. J Immunol. 2000. PMID: 11067932
-
T-cell adoptive therapy of tumors: mechanisms of improved therapeutic performance.Crit Rev Immunol. 2001;21(1-3):215-48. Crit Rev Immunol. 2001. PMID: 11642606 Review.
Cited by
-
STAT3- and STAT5-dependent pathways competitively regulate the pan-differentiation of CD34pos cells into tumor-competent dendritic cells.Blood. 2008 Sep 1;112(5):1832-43. doi: 10.1182/blood-2007-12-130138. Epub 2008 Jun 24. Blood. 2008. PMID: 18577706 Free PMC article.
-
Expansion of melanoma-specific T cells from lymph nodes of patients in stage III: implications for adoptive immunotherapy in treating cancer.Surgery. 2012 Oct;152(4):557-65; discussion 565-6. doi: 10.1016/j.surg.2012.07.002. Epub 2012 Aug 25. Surgery. 2012. PMID: 22925133 Free PMC article.
-
Adoptive transfer of vaccine-induced peripheral blood mononuclear cells to patients with metastatic melanoma following lymphodepletion.J Immunol. 2006 Nov 1;177(9):6527-39. doi: 10.4049/jimmunol.177.9.6527. J Immunol. 2006. PMID: 17056585 Free PMC article. Clinical Trial.
-
Augmented lymphocyte expansion from solid tumors with engineered cells for costimulatory enhancement.J Immunother. 2011 Nov-Dec;34(9):651-61. doi: 10.1097/CJI.0b013e31823284c3. J Immunother. 2011. PMID: 21989413 Free PMC article.
-
An adaptive dose-finding design based on both safety and immunologic responses in cancer clinical trials.Stat Biopharm Res. 2018;10(3):185-195. doi: 10.1080/19466315.2018.1462727. Epub 2018 Apr 30. Stat Biopharm Res. 2018. PMID: 30524665 Free PMC article.
References
-
- Cohen PA, Peng L, Kjaergaard J, et al. T-cell adoptive therapy of tumors: mechanisms of improved therapeutic performance. Crit Rev Immunol. 2001;21:215–248. - PubMed
-
- Rosenberg SA, Packard BS, Aebersold PM, et al. Use of tumor-infiltrating lymphocytes and interleukin-2 in the immunotherapy of patients with metastatic melanoma. N Eng J Med. 1988;319:1676–1680. - PubMed
-
- Yee C, Thompson JA, Byrd D, et al. Adoptive T cell therapy using antigen-specific CD8+ T cell clones for the treatment of patients with metastatic melanoma: in vivo persistence, migration, and antitumor effect of transferred T cells. Proc Natl Acad Sci U S A. 2002;99:16168–16173. doi: 10.1073/pnas.242600099. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

