Clinical review: biphasic positive airway pressure and airway pressure release ventilation
- PMID: 15566621
- PMCID: PMC1065046
- DOI: 10.1186/cc2919
Clinical review: biphasic positive airway pressure and airway pressure release ventilation
Abstract
This review focuses on mechanical ventilation strategies that allow unsupported spontaneous breathing activity in any phase of the ventilatory cycle. By allowing patients with the acute respiratory distress syndrome to breathe spontaneously, one can expect improvements in gas exchange and systemic blood flow, based on findings from both experimental and clinical trials. In addition, by increasing end-expiratory lung volume, as occurs when using biphasic positive airway pressure or airway pressure release ventilation, recruitment of collapsed or consolidated lung is likely to occur, especially in juxtadiaphragmatic lung legions. Traditional approaches to mechanical ventilatory support of patients with acute respiratory distress syndrome require adaptation of the patient to the mechanical ventilator using heavy sedation and even muscle relaxation. Recent investigations have questioned the utility of sedation, muscle paralysis and mechanical control of ventilation. Furthermore, evidence exists that lowering sedation levels will decrease the duration of mechanical ventilatory support, length of stay in the intensive care unit, and overall costs of hospitalization. Based on currently available data, we suggest considering the use of techniques of mechanical ventilatory support that maintain, rather than suppress, spontaneous ventilatory effort, especially in patients with severe pulmonary dysfunction.
Figures
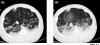
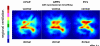


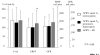
Similar articles
-
Assisted breathing is better in acute respiratory failure.Curr Opin Crit Care. 2005 Feb;11(1):63-8. doi: 10.1097/00075198-200502000-00010. Curr Opin Crit Care. 2005. PMID: 15659947 Review.
-
Airway pressure release and biphasic intermittent positive airway pressure ventilation: are they ready for prime time?J Trauma. 2007 May;62(5):1298-308; discussion 1308-9. doi: 10.1097/TA.0b013e31803c562f. J Trauma. 2007. PMID: 17495742 Review.
-
Patient-ventilator interaction during acute lung injury, and the role of spontaneous breathing: part 2: airway pressure release ventilation.Respir Care. 2011 Feb;56(2):190-203; discussion 203-6. doi: 10.4187/respcare.00968. Respir Care. 2011. PMID: 21333179
-
Pressure control ventilation.Crit Care Clin. 2007 Apr;23(2):183-99, viii-ix. doi: 10.1016/j.ccc.2006.12.005. Crit Care Clin. 2007. PMID: 17368165 Review.
-
Physiologic effects of noninvasive ventilation during acute lung injury.Am J Respir Crit Care Med. 2005 Nov 1;172(9):1112-8. doi: 10.1164/rccm.200402-226OC. Epub 2005 Aug 4. Am J Respir Crit Care Med. 2005. PMID: 16081548
Cited by
-
Airway pressure release ventilation and biphasic positive airway pressure: a systematic review of definitional criteria.Intensive Care Med. 2008 Oct;34(10):1766-73. doi: 10.1007/s00134-008-1216-3. Epub 2008 Jul 17. Intensive Care Med. 2008. PMID: 18633595
-
What on earth is APRV?Crit Care. 2011;15(1):115. doi: 10.1186/cc9419. Epub 2011 Jan 31. Crit Care. 2011. PMID: 21345265 Free PMC article. Review.
-
Airway pressure release ventilation versus assist-control ventilation: a comparative propensity score and international cohort study.Intensive Care Med. 2010 May;36(5):817-27. doi: 10.1007/s00134-010-1837-1. Epub 2010 Mar 13. Intensive Care Med. 2010. PMID: 20229042
-
Complications and Pharmacologic Interventions of Invasive Positive Pressure Ventilation During Critical Illness.J Pharm Technol. 2018 Aug;34(4):153-170. doi: 10.1177/8755122518766594. Epub 2018 Mar 29. J Pharm Technol. 2018. PMID: 34860978 Free PMC article. Review.
-
A narrative review of advanced ventilator modes in the pediatric intensive care unit.Transl Pediatr. 2021 Oct;10(10):2700-2719. doi: 10.21037/tp-20-332. Transl Pediatr. 2021. PMID: 34765495 Free PMC article. Review.
References
-
- Hansen J, Wendt M, Lawin P. A new weaning procedure (inspiratory flow assistance) Anaesthesist. 1984;33:428–432. - PubMed
-
- Younes M. Proportional assist ventilation, a new approach to ventilatory support. Theory. Am Rev Respir Dis. 1992;145:114–120. - PubMed
-
- Downs JB, Klein EF, Jr, Desautels D, Modell JH, Kirby RR. Intermittent mandatory ventilation: a new approach to weaning patients from mechanical ventilators. Chest. 1973;64:331–335. - PubMed
-
- Baum M, Benzer H, Putensen C, Koller W. Biphasic positive airway pressure (BIPAP): a new form of augmented ventilation. Anaesthesist. 1989;38:452–458. - PubMed
-
- Stock MC, Downs JB. Airway pressure release ventilation. Crit Care Med. 1987;15:462–466. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

