Acute methotrexate neurotoxicity: findings on diffusion-weighted imaging and correlation with clinical outcome
- PMID: 15569732
- PMCID: PMC8148738
Acute methotrexate neurotoxicity: findings on diffusion-weighted imaging and correlation with clinical outcome
Abstract
Background and purpose: Acute lymphocytic leukemia (ALL) is a common malignancy of childhood treated with methotrexate (MTX), which is associated with acute neurotoxicity. We evaluated diffusion-weighted (DW) and conventional MR images in children with ALL and acute MTX-induced neurotoxicity, with clinical correlation.
Methods: Five patients aged 12-15 years underwent fluid-attenuated inversion recovery (FLAIR), T2-weighted fast spin-echo and gradient-echo, T1-weighted gadolinium-enhanced spin-echo, and DW imaging within 24 hours of symptom onset. Records were reviewed for the temporal relationship to MTX administration, strokelike symptoms, and neurologic outcome.
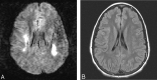
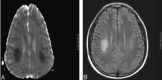
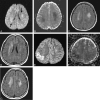
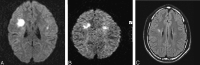
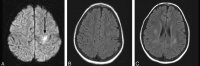
Results: Six strokelike events were temporally related to intrathecal MTX given 6-11 days before symptom onset. FLAIR images showed abnormal hyperintensity in the callosal splenium in one patient but were otherwise normal. Diffusion abnormalities were frontoparietal in three events and frontal in one; nonfluent aphasia was seen in all. Bilateral frontoparietal diffusion abnormalities were associated with bilateral upper-extremity weakness, right-sided hemiparesis, or left-sided hemiparesis (one patient each); one patient had mild facial droop. Unilateral precentral subcortical diffusion abnormality was associated with contralateral motor deficit and ipsilateral upper-extremity sensory loss. Strokelike symptoms resolved rapidly and were not associated with other signs of encephalopathy. Subsequent intrathecal MTX administration was not associated with recurrence in four patients.
Conclusion: Diffusion abnormalities in acute MTX neurotoxicity indicated cerebral dysfunction but not necessarily overt structural injury to the cerebrum. Subsequent demyelination or gliosis could not be predicted on the basis of diffusion abnormalities. A single strokelike episode with diffusion abnormalities should not necessarily prompt modification of potentially curative chemotherapeutic regimens.
Figures
References
-
- Winick NJ, Bowman WP, Kamen BA, et al. Unexpected acute neurologic toxicity in the treatment of children with acute lymphoblastic leukemia. J Natl Cancer Inst 1992;84:252–256 - PubMed
-
- Mahoney DH, Shuster JJ, Nitschke R, et al. Acute neurotoxicity in children with B-precursor acute lymphoid leukemia: an association between intermediate–dose intravenous methotrexate and intrathecal triple therapy: a Pediatric Oncology Group study. J Clin Oncol 1998;16:1712–1722 - PubMed
-
- Winick N, Shuster JJ, Bowman WP, et al. Intensive oral methotrexate protects against lymphoid marrow relapse in childhood B-precursor acute lymphoblastic leukemia. J Clin Oncol 1996;14:2803–2811 - PubMed
-
- Rubnitz JE, Relling MV, Harrison, et al. Transient leukoencephalopathy following high dose methotrexate treatment in childhood acute lymphocytic leukemia. Leukemia 1998;12:1176–1181 - PubMed
-
- Rubinstein LJ, Herman MM, Long TF, Wilbur JR. Disseminated necrotizing leukoencephalopathy: a complication of treated central nervous system leukemia and lymphoma. Cancer 1975;35:291–305 - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
