NHE2-mediated bicarbonate reabsorption in the distal tubule of NHE3 null mice
- PMID: 15604231
- PMCID: PMC1665379
- DOI: 10.1113/jphysiol.2004.074716
NHE2-mediated bicarbonate reabsorption in the distal tubule of NHE3 null mice
Abstract
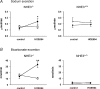
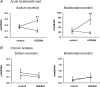
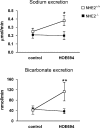
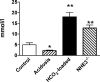
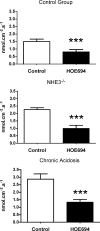
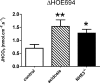
NHE3(-/-) mice display a profound defect in proximal tubule bicarbonate reabsorption but are only mildly acidotic owing to reduced glomerular filtration rate and enhanced H(+) secretion in distal nephron segments. In vivo microperfusion of rat distal tubules suggests that a significant fraction of bicarbonate reabsorption in this nephron segment is mediated by NHE2. Two approaches were used to evaluate the role of distal tubule NHE2 in compensating for the proximal defect of H(+) secretion in NHE3(-/-) mice. First, renal clearance experiments were used to assess the impact of HOE694, an inhibitor with significant affinity for NHE2, on excretion of bicarbonate in NHE3(-/-) and NHE2(-/-) mice. Second, in vivo micropuncture and microperfusion were employed to measure the concentration of bicarbonate in early distal tubule fluid and to measure distal bicarbonate reabsorption during a constant bicarbonate load. Our data show that HOE694 had no effect on urinary bicarbonate excretion in NHE3(+/+) mice, whereas bicarbonate excretion was higher in NHE3(-/-) mice receiving HOE694. HOE694 induced a significant increase in bicarbonate excretion in mice given an acute bicarbonate load, but there was no effect during metabolic acidosis. Bicarbonate excretion was not affected by HOE694 in bicarbonate-loaded NHE2(-/-) mice. In vivo micropuncture revealed that early distal bicarbonate concentration was elevated in both bicarbonate-loaded and NHE3(-/-) mice. Further, microperfusion experiments showed that HOE694-sensitive bicarbonate reabsorption capacity was higher in acidotic and NHE3 null animals. We conclude that NHE2 contributes importantly to acidification in the distal tubule, and that it plays a major role in limiting urinary bicarbonate losses in states in which a high luminal bicarbonate load is presented to the distal tubule, such as in NHE3 null mice.
Figures



Similar articles
-
Role of NHE isoforms in mediating bicarbonate reabsorption along the nephron.Am J Physiol Renal Physiol. 2001 Dec;281(6):F1117-22. doi: 10.1152/ajprenal.2001.281.6.F1117. Am J Physiol Renal Physiol. 2001. PMID: 11704563
-
Mechanism of proximal tubule bicarbonate absorption in NHE3 null mice.Am J Physiol. 1999 Aug;277(2):F298-302. doi: 10.1152/ajprenal.1999.277.2.F298. Am J Physiol. 1999. PMID: 10444585
-
Proximal tubule specific knockout of the Na⁺/H⁺ exchanger NHE3: effects on bicarbonate absorption and ammonium excretion.J Mol Med (Berl). 2013 Aug;91(8):951-63. doi: 10.1007/s00109-013-1015-3. Epub 2013 Mar 19. J Mol Med (Berl). 2013. PMID: 23508938 Free PMC article.
-
Distal tubule bicarbonate transport.J Nephrol. 2002 Mar-Apr;15 Suppl 5:S97-111. J Nephrol. 2002. PMID: 12027226 Review.
-
New Insights into the Critical Importance of Intratubular Na+/H+ Exchanger 3 and Its Potential Therapeutic Implications in Hypertension.Curr Hypertens Rep. 2021 Jun 10;23(6):34. doi: 10.1007/s11906-021-01152-7. Curr Hypertens Rep. 2021. PMID: 34110521 Free PMC article. Review.
Cited by
-
Recording ion channels in isolated, split-opened tubules.Methods Mol Biol. 2013;998:341-53. doi: 10.1007/978-1-62703-351-0_27. Methods Mol Biol. 2013. PMID: 23529443 Free PMC article.
-
H+-ATPase B1 subunit localizes to thick ascending limb and distal convoluted tubule of rodent and human kidney.Am J Physiol Renal Physiol. 2018 Sep 1;315(3):F429-F444. doi: 10.1152/ajprenal.00539.2017. Epub 2018 Jul 11. Am J Physiol Renal Physiol. 2018. PMID: 29993276 Free PMC article.
-
Molecular mechanisms and regulation of urinary acidification.Compr Physiol. 2014 Oct;4(4):1737-74. doi: 10.1002/cphy.c140021. Compr Physiol. 2014. PMID: 25428859 Free PMC article. Review.
-
A switch in the mechanism of hypertension in the syndrome of apparent mineralocorticoid excess.J Am Soc Nephrol. 2008 Jan;19(1):47-58. doi: 10.1681/ASN.2007040401. Epub 2007 Nov 21. J Am Soc Nephrol. 2008. PMID: 18032795 Free PMC article.
-
Na+/H+ exchangers in renal regulation of acid-base balance.Semin Nephrol. 2006 Sep;26(5):334-44. doi: 10.1016/j.semnephrol.2006.07.001. Semin Nephrol. 2006. PMID: 17071327 Free PMC article. Review.
References
-
- Amemiya M, Loffing J, Lotscher M, Kaissling B, Alpern RJ, Moe OW. Expression of NHE3 in the apical membrane of rat renal proximal tubule and thick ascending limb. Kidney Int. 1995;48:1206–1215. - PubMed
-
- Amorim JB, Bailey MA, Musa-Aziz R, Giebisch G, Malnic G. Role of luminal anion and pH in distal tubule potassium secretion. Am J Physiol Renal Physiol. 2003;284:F381–F388. - PubMed
-
- Bailey MA. Inhibition of bicarbonate reabsorption in the rat proximal tubule by activation of luminal P2Y1 receptors. Am J Physiol Renal Physiol. 2004;287:F789–F796. - PubMed
-
- Berliner RW, Kennedy TJ. Renal tubular secretion of potassium in the normal dog. Proc Soc Exper Biol Medical. 1948;67:542–545. - PubMed
-
- Biemesderfer D, Reilly RF, Exner M, Igarashi P, Aronson PS. Immunocytochemical characterization of Na+-H+ exchanger isoform NHE-1 in rabbit kidney. Am J Physiol. 1992;263:F833–F840. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Molecular Biology Databases

