The prognosis of women with stage IB1-IIB node-positive cervical carcinoma after radical surgery
- PMID: 15606922
- PMCID: PMC546224
- DOI: 10.1186/1477-7819-2-47
The prognosis of women with stage IB1-IIB node-positive cervical carcinoma after radical surgery
Abstract
Background: Pelvic lymph nodes metastasis is an important prognostic factor for patients with cervical carcinoma. However, the relationships between the number of positive nodes, site of metastases nodes, adjuvant therapy and the prognosis is controversial. The purpose of this study was to investigate the influence of positive lymph nodes on the prognosis of Chinese women with stage IB1-IIB cervical carcinoma.
Patients and methods: Between January 1992 and December 1997, 398 women with International Federation of Gynecology and Obstetrics (FIGO) stage IB1-IIB cervical carcinoma underwent radical surgery in Cancer Hospital, Fudan University. Of these sixty-six patients (16.6%) who were histologically confirmed to have positive pelvic lymph nodes were analyzed retrospectively. The survival was estimated using Kaplan-Meier method. The differences in survival were compared with Log-rank test. Multivariate analyses were performed with the Cox proportional hazard model.
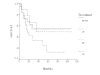
Results: The 5-year survival of the patients with pelvic lymph nodes metastases was 40.7%. Cox proportional hazard model analysis showed that cellular differentiation, the number of positive nodes and adjuvant therapy to be the independent prognostic factors (P < 0.05). The 5-year survival of patients with one positive node was higher than that of those with two or more positive nodes (56.5% vs. 36.4%, P < 0.05). The distant metastasis rate in the former group (5.9%) was lower than the latter's (32.7%) (P = 0.05). However, there was no significant difference of pelvic recurrence between the two groups (P > 0.05). The number of positive nodes positively correlated with the level of positive nodes (P < 0.01). The 5-year survival of the patients who had no adjuvant therapy (12.6%) was much lower than that (53.7%) of those with adjuvant therapy (P < 0.05). However, there was no obvious difference between adjuvant radiotherapy, chemotherapy and chemo-radiotherapy (P > 0.05).
Conclusions: The prognosis of patients with stage IB1-IIB node-positive cervical carcinoma who underwent radical surgery alone was very poor. Adjuvant therapy increases the survival rate, decreases the pelvic recurrence and distant metastasis.
Figures
Similar articles
-
[Prognosis of patients with stage Ib-IIb node-positive cervical carcinoma].Ai Zheng. 2003 Nov;22(11):1219-23. Ai Zheng. 2003. PMID: 14613657 Chinese.
-
Lymph-vascular space invasion and number of positive para-aortic node groups predict survival in node-positive patients with endometrial cancer.Gynecol Oncol. 2005 Mar;96(3):651-7. doi: 10.1016/j.ygyno.2004.11.026. Gynecol Oncol. 2005. PMID: 15721407
-
[Effects of pre-chemotherapy hemoglobin and platelet levels in patients with stage Ib2-IIb cervical cancer treated with neoadjuvant chemotherapy followed by radical hysterectomy].Zhonghua Fu Chan Ke Za Zhi. 2012 Aug;47(8):577-81. Zhonghua Fu Chan Ke Za Zhi. 2012. PMID: 23141176 Chinese.
-
Adenosquamous histology predicts a poor outcome for patients with advanced-stage, but not early-stage, cervical carcinoma.Cancer. 2003 May 1;97(9):2196-202. doi: 10.1002/cncr.11371. Cancer. 2003. PMID: 12712471 Review.
-
The Effect of Neoadjuvant Chemotherapy on Lymph Node Metastasis of FIGO Stage IB1-IIB Cervical Cancer: A Systematic Review and Meta-Analysis.Front Oncol. 2020 Nov 5;10:570258. doi: 10.3389/fonc.2020.570258. eCollection 2020. Front Oncol. 2020. PMID: 33251136 Free PMC article.
Cited by
-
Survival and prognosticators of node-positive cervical cancer patients treated with radical hysterectomy and systematic lymphadenectomy.Int J Clin Oncol. 2011 Feb;16(1):33-8. doi: 10.1007/s10147-010-0123-0. Epub 2010 Sep 15. Int J Clin Oncol. 2011. PMID: 20842404
-
Imaging in Carcinoma Cervix and Revised 2018 FIGO Staging System: Implications in Radiology Reporting.Indian J Radiol Imaging. 2021 Sep 7;31(3):623-634. doi: 10.1055/s-0041-1735502. eCollection 2021 Jul. Indian J Radiol Imaging. 2021. PMID: 34790308 Free PMC article. Review.
-
Parametrial involvement and decreased survival of women with FIGO stage IIIC1 cervical cancer.J Gynecol Oncol. 2023 Jul;34(4):e46. doi: 10.3802/jgo.2023.34.e46. Epub 2023 Mar 13. J Gynecol Oncol. 2023. PMID: 36929577 Free PMC article.
-
Current Paradigm and Future Directions in the Management of Nodal Disease in Locally Advanced Cervical Cancer.Cancers (Basel). 2025 Jan 9;17(2):202. doi: 10.3390/cancers17020202. Cancers (Basel). 2025. PMID: 39857985 Free PMC article. Review.
-
Development of a Deep Learning Model to Identify Lymph Node Metastasis on Magnetic Resonance Imaging in Patients With Cervical Cancer.JAMA Netw Open. 2020 Jul 1;3(7):e2011625. doi: 10.1001/jamanetworkopen.2020.11625. JAMA Netw Open. 2020. PMID: 32706384 Free PMC article.
References
-
- Monk BJ, Cha DS, Walker JL, Burger RA, Ramsinghani NS, Manetta A, Disaia PJ, Berman ML. Extent of disease as an indication for pelvic radiation following radical hysterectomy and bilateral pelvic lymph node dissection in the treatment of stage IB and IIA cervical carcinoma. Gynecol Oncol. 1994;54:4–9. doi: 10.1006/gyno.1994.1157. - DOI - PubMed
-
- Hopkins MP, Morley GW. Stage Ib squamous cell cancer of the cervix: Clinicopathologic features related to survival. Am J Obstet Gynecol. 1991;164:1520–1527. - PubMed
-
- Hsu CT, Cheng YS, Su SC. Prognosis of uterine cervical cancer with extensive lymph node metastases: Special emphasis on the value of pelvic lymphadenectomy in the surgical treatment of uterine cervical cancer. Am J Obstet Gynecol. 1972;114:954–962. - PubMed
-
- Inoue T, Morita K. The prognostic significance of number of positive nodes in cervical carcinoma stage Ib, IIa, IIb. Cancer. 1990;65:1923–1927. - PubMed
-
- Lanza A, Re A, Daddato F, Raspollini M, Proserpio D, Bellino R, Morino M, Ferraris G. Treatment failure in cervical cancer: High risk features of relapse. Eur J Gynaecol Oncol. 1989;10:326–336. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources