Focal hyperhidrosis: diagnosis and management
- PMID: 15632408
- PMCID: PMC543948
- DOI: 10.1503/cmaj.1040708
Focal hyperhidrosis: diagnosis and management
Abstract
Hyperhidrosis, a condition characterized by excessive sweating, can be generalized or focal. Generalized hyperhidrosis involves the entire body and is usually part of an underlying condition, most often an infectious, endocrine or neurologic disorder. Focal hyperhidrosis is idiopathic, occurring in otherwise healthy people. It affects 1 or more body areas, most often the palms, armpits, soles or face. Almost 3% of the general population, largely people aged between 25 and 64 years, experience hyperhidrosis. The condition carries a substantial psychological and social burden, since it interferes with daily activities. However, patients rarely seek a physician's help because many are unaware that they have a treatable medical disorder. Early detection and management of hyperhidrosis can significantly improve a patient's quality of life. There are various topical, systemic, surgical and nonsurgical treatments available with efficacy rates greater than 90%-95%.
Figures


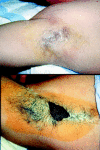



References
-
- Amir M, Arish A, Weinstein Y, Pfeffer M, Levy Y. Impairment in quality of life among patients seeking surgery for hyperhidrosis (excessive sweating): preliminary results. Isr J Psychiatry Relat Sci 2000;37(1):25-31. - PubMed
-
- Lerer B, Jacobowitz J, Wahaba A. Personality features in essential hyperhidrosis. Int J Psychiatry Med 1981;10:59-67. - PubMed
-
- Christophers E, Kruger G. Psoriasis. In: Fitzpatrick TB, Eisen AZ, Wolff K, editors. Dermatology in general medicine. 3rd ed. New York: McGraw-Hill; 1987. p. 465.
-
- Strutton DR, Kowalski JW, Glaser DA, Stang PE. US prevalence of hyperhidrosisand impact on individuals with axillary hyperhidrosis: Results from a national survey. J Am Acad Dermatol 2004;51(2):241-8. - PubMed
-
- Lin TS, Fang HY. Transthoracic endoscopic sympathectomy in the treatment of palmar hyperhidrosis — with emphasis on perioperative management (1360 case analysis). Surg Neurol 1999;52:453-7. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
