Bloodstream infections caused by antibiotic-resistant gram-negative bacilli: risk factors for mortality and impact of inappropriate initial antimicrobial therapy on outcome
- PMID: 15673761
- PMCID: PMC547233
- DOI: 10.1128/AAC.49.2.760-766.2005
Bloodstream infections caused by antibiotic-resistant gram-negative bacilli: risk factors for mortality and impact of inappropriate initial antimicrobial therapy on outcome
Abstract
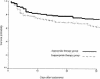
The marked increase in the incidence of infections due to antibiotic-resistant gram-negative bacilli in recent years is of great concern, as patients infected by those isolates might initially receive antibiotics that are inactive against the responsible pathogens. To evaluate the effect of inappropriate initial antimicrobial therapy on survival, a total of 286 patients with antibiotic-resistant gram-negative bacteremia, 61 patients with Escherichia coli bacteremia, 65 with Klebsiella pneumoniae bacteremia, 74 with Pseudomonas aeruginosa bacteremia, and 86 with Enterobacter bacteremia, were analyzed retrospectively. If a patient received at least one antimicrobial agent to which the causative microorganisms were susceptible within 24 h of blood culture collection, the initial antimicrobial therapy was considered to have been appropriate. High-risk sources of bacteremia were defined as the lung, peritoneum, or an unknown source. The main outcome measure was 30-day mortality. Of the 286 patients, 135 (47.2%) received appropriate initial empirical antimicrobial therapy, and the remaining 151 (52.8%) patients received inappropriate therapy. The adequately treated group had a 27.4% mortality rate, whereas the inadequately treated group had a 38.4% mortality rate (P = 0.049). Multivariate analysis showed that the significant independent risk factors of mortality were presentation with septic shock, a high-risk source of bacteremia, P. aeruginosa infection, and an increasing APACHE II score. In the subgroup of patients (n = 132) with a high-risk source of bacteremia, inappropriate initial antimicrobial therapy was independently associated with increased mortality (odds ratio, 3.64; 95% confidence interval, 1.13 to 11.72; P = 0.030). Our data suggest that inappropriate initial antimicrobial therapy is associated with adverse outcome in antibiotic-resistant gram-negative bacteremia, particularly in patients with a high-risk source of bacteremia.
Figures
Comment in
-
Impact of initial antimicrobial therapy in patients with bloodstream infections caused by Stenotrophomonas maltophilia.Antimicrob Agents Chemother. 2005 Sep;49(9):3980-1. doi: 10.1128/AAC.49.9.3980-3981.2005. Antimicrob Agents Chemother. 2005. PMID: 16127088 Free PMC article. No abstract available.
References
-
- Bates, D. W., K. E. Pruess, and T. H. Lee. 1995. How bad are bacteremia and sepsis? Outcomes in a cohort with suspected bacteremia. Arch. Intern. Med. 155:593-598. - PubMed
-
- Blot, S., K. Vandewoude, D. De Bacquer, and F. Colardyn. 2002. Nosocomial bacteremia caused by antibiotic-resistant gram-negative bacteria in critically ill patients: clinical outcome and length of hospitalization. Clin. Infect. Dis. 34:1600-1606. - PubMed
-
- Cosgrove, S. E., K. S. Kaye, G. M. Eliopoulous, and Y. Carmeli. 2002. Health and economic outcomes of the emergence of third-generation cephalosporin resistance in Enterobacter species. Arch. Intern. Med. 162:185-190. - PubMed
-
- Garner, J. S., W. R. Jarvis, T. G. Emori, T. C. Horan, and J. M. Hughes. 1988. CDC definitions for nosocomial infections. Am. J. Infect. Control 16:128-140. - PubMed
-
- Hanon, F. X., D. L. Monnet, T. L. Sorensen, K. Molbak, G. Pedersen, and H. Schonheyder. 2002. Survival of patients with bacteraemia in relation to initial empirical antimicrobial treatment. Scand. J. Infect. Dis. 34:520-528. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

