Autoregulation of the cerebral circulation during sleep in newborn lambs
- PMID: 15760939
- PMCID: PMC1464469
- DOI: 10.1113/jphysiol.2005.083352
Autoregulation of the cerebral circulation during sleep in newborn lambs
Abstract
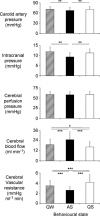
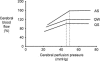
Autoregulation is a vital protective mechanism that maintains stable cerebral blood flow as cerebral perfusion pressure changes. We contrasted cerebral autoregulation across sleep-wake states, as little is known about its effectiveness during sleep. Newborn lambs (n= 9) were instrumented to measure cerebral blood flow (flow probe on the superior sagittal sinus) and cerebral perfusion pressure, then studied during active sleep (AS), quiet sleep (QS) and quiet wakefulness (QW). We generated cerebral autoregulation curves by inflating an occluder cuff around the brachiocephalic artery thereby lowering cerebral perfusion pressure. Baseline cerebral blood flow was higher (P < 0.05) and cerebral vascular resistance lower (P < 0.05) in AS than in QW (76 +/- 8% and 133 +/- 15%, respectively, of the AS value, mean +/-s.d.) and in QS (66 +/- 11% and 158 +/- 30%). The autoregulation curve in AS differed from that in QS and QW in three key respects: firstly, the plateau was elevated relative to QS and QW (P < 0.05); secondly, the lower limit of the curve (breakpoint) was higher (P < 0.05) in AS (50 mmHg) than QS (45 mmHg); and thirdly, the slope of the descending limb below the breakpoint was greater (P < 0.05) in AS than QS (56% of AS) or QW (56% of AS). Although autoregulation functions in AS, the higher breakpoint and greater slope of the descending limb may place the brain at risk for vascular compromise should hypotension occur.
Figures


Similar articles
-
Cerebral circulation in sleep: vasodilatory response to cerebral hypotension.J Cereb Blood Flow Metab. 1998 Jun;18(6):639-45. doi: 10.1097/00004647-199806000-00006. J Cereb Blood Flow Metab. 1998. PMID: 9626188
-
Sympathetic nervous control of the cerebral circulation in sleep.J Sleep Res. 2005 Sep;14(3):275-83. doi: 10.1111/j.1365-2869.2005.00464.x. J Sleep Res. 2005. PMID: 16120102
-
Cerebral sympathetic nerve activity has a major regulatory role in the cerebral circulation in REM sleep.J Appl Physiol (1985). 2009 Apr;106(4):1050-6. doi: 10.1152/japplphysiol.91349.2008. Epub 2009 Jan 15. J Appl Physiol (1985). 2009. PMID: 19150858
-
Transcranial Doppler assessment of cerebral autoregulation.Ultrasound Med Biol. 2009 Jun;35(6):883-93. doi: 10.1016/j.ultrasmedbio.2009.01.005. Epub 2009 Mar 28. Ultrasound Med Biol. 2009. PMID: 19329245 Review.
-
The critical closing pressure of the cerebral circulation.Med Eng Phys. 2003 Oct;25(8):621-32. doi: 10.1016/s1350-4533(03)00027-4. Med Eng Phys. 2003. PMID: 12900178 Review.
Cited by
-
Assessment of MR blood-oxygen-level-dependent (BOLD) cerebrovascular reactivity under general anesthesia in children with moyamoya.Pediatr Radiol. 2024 Jul;54(8):1325-1336. doi: 10.1007/s00247-024-05930-8. Epub 2024 May 23. Pediatr Radiol. 2024. PMID: 38777883
-
Obstructive sleep apnea leads to transient uncoupling of coronary blood flow and myocardial work in humans.Sleep. 2009 Feb;32(2):263-70. doi: 10.1093/sleep/32.2.263. Sleep. 2009. PMID: 19238814 Free PMC article.
-
Fetal cerebral blood flow, electrocorticographic activity, and oxygenation: responses to acute hypoxia.J Physiol. 2009 May 1;587(Pt 9):2033-47. doi: 10.1113/jphysiol.2009.166983. J Physiol. 2009. PMID: 19406885 Free PMC article.
-
Early Changes in Glutamate Metabolism and Perfusion in Basal Ganglia following Hypoxia-Ischemia in Neonatal Piglets: A Multi-Sequence 3.0T MR Study.Front Physiol. 2017 Apr 25;8:237. doi: 10.3389/fphys.2017.00237. eCollection 2017. Front Physiol. 2017. PMID: 28487658 Free PMC article.
-
Cerebrovascular control is altered in healthy term infants when they sleep prone.Sleep. 2013 Dec 1;36(12):1911-8. doi: 10.5665/sleep.3228. Sleep. 2013. PMID: 24293766 Free PMC article.
References
-
- Baker SB, Fewell JE. Heart rate response to arousal and lung inflation following upper airway obstruction in lambs. Sleep. 1988;11:233–241. - PubMed
-
- Chamorro A, Vila N, Ascaso C, Elices E, Schonewille W, Blanc R. Blood pressure and functional recovery in acute ischemic stroke. Stroke. 1998;29:1850–1853. - PubMed
-
- Chillon J-M, Baumbach GL. Autoregulation: arterial and intracranial pressure. In: Edvinsson L, Krause DN, editors. Cerebral Blood Flow and Metabolism. Philadelphia: Lippincott. Williams & Wilkins; 2002. pp. 395–412.
-
- Cianci T, Zoccoli G, Lenzi P, Franzini C. Loss of integrative control of peripheral circulation during desynchronized sleep. Am J Physiol Regul Integr Comp Physiol. 1991;261:R373–R377. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Research Materials

