Hemodialysis in children: general practical guidelines
- PMID: 15947992
- PMCID: PMC1766474
- DOI: 10.1007/s00467-005-1876-y
Hemodialysis in children: general practical guidelines
Abstract
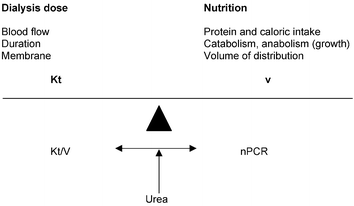
Over the past 20 years children have benefited from major improvements in both technology and clinical management of dialysis. Morbidity during dialysis sessions has decreased with seizures being exceptional and hypotensive episodes rare. Pain and discomfort have been reduced with the use of chronic internal jugular venous catheters and anesthetic creams for fistula puncture. Non-invasive technologies to assess patient target dry weight and access flow can significantly reduce patient morbidity and health care costs. The development of urea kinetic modeling enables calculation of the dialysis dose delivery, Kt/V, and an indirect assessment of the intake. Nutritional assessment and support are of major importance for the growing child. Even if the validity of these "urea only" data is questioned, their analysis provides information useful for follow-up. Newer machines provide more precise control of ultrafiltration by volumetric assessment and continuous blood volume monitoring during dialysis sessions. Buffered bicarbonate solutions are now standard and more biocompatible synthetic membranes and specific small size material dialyzers and tubing have been developed for young infants. More recently, the concept of "ultrapure" dialysate, i.e. free from microbiological contamination and endotoxins, has developed. This will enable the use of hemodiafiltration, especially with the on-line option, which has many theoretical advantages and should be considered in the case of maximum/optimum dialysis need. Although the optimum dialysis dose requirement for children remains uncertain, reports of longer duration and/or daily dialysis show they are more effective for phosphate control than conventional hemodialysis and should be considered at least for some high-risk patients with cardiovascular impairment. In children hemodialysis has to be individualized and viewed as an "integrated therapy" considering their long-term exposure to chronic renal failure treatment. Dialysis is seen only as a temporary measure for children compared with renal transplantation because this enables the best chance of rehabilitation in terms of educational and psychosocial functioning. In long term chronic dialysis, however, the highest standards should be applied to these children to preserve their future "cardiovascular life" which might include more dialysis time and on-line hemodiafiltration with synthetic high flux membranes if we are able to improve on the rather restricted concept of small-solute urea dialysis clearance.
References
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '11865081', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/11865081/'}]}
- Fischbach M, Stefanidis CJ, Watson AR (2002) Guidelines by an ad hoc European committee on adequacy of the pediatric peritoneal dialysis prescription. Nephrol Dial Transplant 17:380–385 - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PMC', 'value': 'PMC1766478', 'is_inner': False, 'url': 'https://pmc.ncbi.nlm.nih.gov/articles/PMC1766478/'}, {'type': 'PubMed', 'value': '14685840', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/14685840/'}]}
- Strazdins V, Stefanidis V, Watson AR, Harvey B (2004) Renal replacement therapy for acute renal failure in children: European guidelines. Pediatr Nephrol 19:199–207 - PMC - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '11559888', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/11559888/'}]}
- Fischbach M, Terzic J, Menouer S, Provot E, Bergere V (2001) Hemodialysis in children: principles and practice. Semin Nephrol 21:470–479 - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PMC', 'value': 'PMC1766475', 'is_inner': False, 'url': 'https://pmc.ncbi.nlm.nih.gov/articles/PMC1766475/'}, {'type': 'PubMed', 'value': '16247644', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/16247644/'}]}
- Watson AR, Thurlby D, Schröder C, Fischbach M, Schaefer F, Edefonti A, Stefanidis CJ, Rönnholm K, Zurowska A (2000) Choice of end stage renal failure therapy in eight European centres. Pediatr Nephrol 6(5):C38 - PMC - PubMed
-
- {'text': '', 'ref_index': 1, 'ids': [{'type': 'PubMed', 'value': '7819005', 'is_inner': True, 'url': 'https://pubmed.ncbi.nlm.nih.gov/7819005/'}]}
- Feber J, Scharer K, Schaefer F, Mikova M, Janda J (1994) Residual renal function in children on haemodialysis and peritoneal dialysis therapy. Pediatr Nephrol 8:579–583 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous