The prescribing of methadone and other opioids to addicts: national survey of GPs in England and Wales
- PMID: 15970068
- PMCID: PMC1472740
The prescribing of methadone and other opioids to addicts: national survey of GPs in England and Wales
Abstract
Background: GPs occupy a pivotal position in relation to providing services to opiate misusers in the UK, and this is now cited to support initiatives in other countries.
Aims: To investigate GP involvement in the management of opiate misusers; and to examine the nature of this prescribing of methadone and other opioids.
Design: GP data collected via self-completion postal questionnaire from a 10% random sample of the 30 000 GPs across England and Wales. Patient prescription data obtained on opiate misusers treated during the preceding 4 weeks.
Setting: Primary healthcare practice in England and Wales in mid-2001.
Method: A questionnaire was mailed to a random 10% sample of GPs stratified by number of partners in the practice, with three follow-up mailshots. Data on drugs prescribed by these practitioners were also studied, including drug prescribed, form, dose and dispensing arrangements.
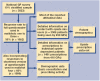
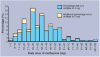
Results: The response rate was 66%. Opiate misusers had been seen by 51% of GPs in the preceding 4 weeks (mean of 4.1 such patients), of whom 50% had prescribed opiate-substitution drugs. This provided a study sample of 1482 opiate misusers to whom GPs were prescribing methadone (86.7%), dihydrocodeine (8.5%) or buprenorphine (4.4%). Of 1292 methadone prescriptions, mean daily dose was 36.9 mg - 47.9% being for 30 mg or less. Daily interval dispensing was stipulated by 44.6%, while 42.9% permitted weekly take-away supply.
Conclusions: In 2001 nearly three times as many GPs were seeing opiate misusers than was the case in 1985. Half were prescribing substitute-opiate drugs such as methadone (to an estimated 30 000 patients). However, there are grounds for concern about the quality of this prescribing. Most doses were too low to constitute optimal methadone maintenance; widespread disregard of the availability of supervised or interval dispensing increases the risks of diversion to the blackmarket and deaths from methadone overdose. Increased quantity of care has been achieved. Increased quality is now required.
Figures

Comment in
-
Treating addiction.Br J Gen Pract. 2005 Jul;55(516):558. Br J Gen Pract. 2005. PMID: 16004755 Free PMC article. No abstract available.
-
Prescribing to substance misusers.Br J Gen Pract. 2005 Aug;55(517):638. Br J Gen Pract. 2005. PMID: 16105377 Free PMC article. No abstract available.
Similar articles
-
Does prescribing for opiate addiction change after national guidelines? Methadone and buprenorphine prescribing to opiate addicts by general practitioners and hospital doctors in England, 1995-2005.Addiction. 2007 May;102(5):761-70. doi: 10.1111/j.1360-0443.2007.01762.x. Addiction. 2007. PMID: 17506153
-
Prescribing injectable and oral methadone to opiate addicts: results from the 1995 national postal survey of community pharmacies in England and Wales.BMJ. 1996 Aug 3;313(7052):270-2. doi: 10.1136/bmj.313.7052.270. BMJ. 1996. PMID: 8704540 Free PMC article.
-
Deaths of opiate/opioid misusers involving dihydrocodeine, UK, 1997-2007.Br J Clin Pharmacol. 2011 Aug;72(2):330-7. doi: 10.1111/j.1365-2125.2011.03908.x. Br J Clin Pharmacol. 2011. PMID: 21235617 Free PMC article.
-
Opioids and the management of chronic severe pain in the elderly: consensus statement of an International Expert Panel with focus on the six clinically most often used World Health Organization Step III opioids (buprenorphine, fentanyl, hydromorphone, methadone, morphine, oxycodone).Pain Pract. 2008 Jul-Aug;8(4):287-313. doi: 10.1111/j.1533-2500.2008.00204.x. Epub 2008 May 23. Pain Pract. 2008. PMID: 18503626
-
Opioid epidemic in the United States.Pain Physician. 2012 Jul;15(3 Suppl):ES9-38. Pain Physician. 2012. PMID: 22786464 Review.
Cited by
-
Diagnosing and managing prescription opioid use disorder in patients prescribed opioids for chronic pain in Australian general practice settings: a qualitative study using the theory of Planned Behaviour.BMC Prim Care. 2024 Jul 3;25(1):236. doi: 10.1186/s12875-024-02474-6. BMC Prim Care. 2024. PMID: 38961328 Free PMC article.
-
Prescribing to substance misusers.Br J Gen Pract. 2005 Aug;55(517):638. Br J Gen Pract. 2005. PMID: 16105377 Free PMC article. No abstract available.
-
Prescribing to substance misusers. Letter response.Br J Gen Pract. 2006 Apr;56(525):301-2. Br J Gen Pract. 2006. PMID: 16611521 Free PMC article. No abstract available.
-
Comparison of methadone and buprenorphine for opiate detoxification (LEEDS trial): a randomised controlled trial.Br J Gen Pract. 2011 Dec;61(593):e772-80. doi: 10.3399/bjgp11X613106. Br J Gen Pract. 2011. PMID: 22137413 Free PMC article. Clinical Trial.
-
Retention of opioid agonist treatment prescribers across New South Wales, Australia, 2001-2018: Implications for treatment systems and potential impact on client outcomes.Drug Alcohol Depend. 2021 Feb 1;219:108464. doi: 10.1016/j.drugalcdep.2020.108464. Epub 2020 Dec 19. Drug Alcohol Depend. 2021. PMID: 33360851 Free PMC article.
References
-
- Department of Health. The New NHS: modern, dependable. London: The Stationery Office; 1997.
-
- Farrar M. Primary care trusts: establishing better services. London: NHS Executive; 1999. http://www.dh.gov.uk/assetRoot/04/05/72/10/04057210.pdf (accessed 27 April 2005)
-
- Department of Heath. The NHS Plan: a plan for investment, a plan for reform. London: The Stationery Office; 2000. http://www.dh.gov.uk/assetRoot/04/05/57/83/040557.pdf (accessed 27 April 2005)
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
