Toll-like receptor 2 expression is decreased on alveolar macrophages in cigarette smokers and COPD patients
- PMID: 16004610
- PMCID: PMC1187924
- DOI: 10.1186/1465-9921-6-68
Toll-like receptor 2 expression is decreased on alveolar macrophages in cigarette smokers and COPD patients
Abstract
Background: Cigarette smoke exposure including biologically active lipopolysaccharide (LPS) in the particulate phase of cigarette smoke induces activation of alveolar macrophages (AM) and alveolar epithelial cells leading to production of inflammatory mediators. This represents a crucial mechanism in the pathogenesis of chronic obstructive pulmonary disease (COPD). Respiratory pathogens are a major cause of exacerbations leading to recurrent cycles of injury and repair. The interaction between pathogen-associated molecular patterns and the host is mediated by pattern recognition receptors (PRR's). In the present study we characterized the expression of Toll-like receptor (TLR)- 2, TLR4 and CD14 on human AM compared to autologous monocytes obtained from patients with COPD, healthy smokers and non-smokers.
Methods: The study population consisted of 14 COPD patients without evidence for acute exacerbation, 10 healthy smokers and 17 healthy non-smokers stratified according to age. The expression of TLR2, TLR4 and CD14 surface molecules on human AM compared to autologous monocytes was assessed ex vivo using FACS analysis. In situ hybridization was performed on bronchoalveolar lavage (BAL) cells by application of the new developed HOPE-fixative.
Results: The expression of TLR2, TLR4 and CD14 on AM from COPD patients, smokers and non-smokers was reduced as compared to autologous monocytes. Comparing AM we detected a reduced expression of TLR2 in COPD patients and smokers. In addition TLR2 mRNA and protein expression was increased after LPS stimulation on non-smokers AM in contrast to smokers and COPD patients.
Conclusion: Our data suggest a smoke related change in the phenotype of AM's and the cellular response to microbial stimulation which may be associated with impairment of host defenses in the lower respiratory tract.
Figures
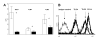
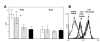

References
-
- Prieto A, Reyes E, Bernstein ED, Martinez B, Monserrat J, Izquierdo JL, Callol L, de Lucas P, Alvarez-Sala R, Alvarez-Sala JL, Villarrubia VG, Alvarez-Mon M. Defective natural killer and phagocytic activities in chronic obstructive pulmonary disease are restored by glycophosphopeptical (inmunoferon) Am J Respir Crit Care Med. 2001;163:1578–1583. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

