Endothelial cell injury by high glucose and heparanase is prevented by insulin, heparin and basic fibroblast growth factor
- PMID: 16086844
- PMCID: PMC1192813
- DOI: 10.1186/1475-2840-4-12
Endothelial cell injury by high glucose and heparanase is prevented by insulin, heparin and basic fibroblast growth factor
Abstract
Background: Uncontrolled hyperglycemia is the main risk factor in the development of diabetic vascular complications. The endothelial cells are the first cells targeted by hyperglycemia. The mechanism of endothelial injury by high glucose is still poorly understood. Heparanase production, induced by hyperglycemia, and subsequent degradation of heparan sulfate may contribute to endothelial injury. Little is known about endothelial injury by heparanase and possible means of preventing this injury.
Objectives: To determine if high glucose as well as heparanase cause endothelial cell injury and if insulin, heparin and bFGF protect cells from this injury.
Methods: Cultured porcine aortic endothelial cells were treated with high glucose (30 mM) and/or insulin (1 U/ml) and/or heparin (0.5 microg/ml) and /or basic fibroblast growth factor (bFGF) (1 ng/ml) for seven days. Cells were also treated with heparinase I (0.3 U/ml, the in vitro surrogate heparanase), plus insulin, heparin and bFGF for two days in serum free medium. Endothelial cell injury was evaluated by determining the number of live cells per culture and lactate dehydrogenase (LDH) release into medium expressed as percentage of control.
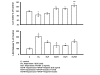
Results: A significant decrease in live cell number and increase in LDH release was found in endothelial cells treated with high glucose or heparinase I. Insulin and/or heparin and/or bFGF prevented these changes and thus protected cells from injury by high glucose or heparinase I. The protective ability of heparin and bFGF alone or in combination was more evident in cells damaged with heparinase I than high glucose.
Conclusion: Endothelial cells injured by high glucose or heparinase I are protected by a combination of insulin, heparin and bFGF, although protection by heparin and/or bFGF was variable.
Figures




References
-
- Ruderman NB, Williamson JR, Brownlee M. Glucose and diabetic vascular disease. FASEB J. 1992;6:2905–2914. - PubMed
-
- Aiello LP, Avery RL, Arrigg PG, Keyt BA, Jampel HD, Shah ST, Pasquale LR, Thieme H, Iwamoto MA, Park JE, . Vascular endothelial growth factor in ocular fluid of patients with diabetic retinopathy and other retinal disorders 2. N Engl J Med. 1994;331:1480–1487. doi: 10.1056/NEJM199412013312203. - DOI - PubMed
-
- Mogensen CE, Schmitz A, Christensen CK. Comparative renal pathophysiology relevant to IDDM and NIDDM patients 5. Diabetes Metab Rev. 1988;4:453–483. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

