Preventing prolonged post-operative ileus in gastric cancer patients undergoing gastrectomy and intra-peritoneal chemotherapy
- PMID: 16097043
- PMCID: PMC4398721
- DOI: 10.3748/wjg.v11.i31.4776
Preventing prolonged post-operative ileus in gastric cancer patients undergoing gastrectomy and intra-peritoneal chemotherapy
Abstract
Aim: To assess the efficacy of metoclopramide (Met) for prevention of prolonged post-operative ileus in advanced gastric cancer patients undergoing D2 gastrectomy and intra-peritoneal chemotherapy (IPC).
Methods: Thirty-two advanced gastric cancer patients undergoing D2 gastrectomy and IPC were allocated to two groups. Sixteen patients received Met immediately after operation (group A), and 16 did not (group B). Another 16 patients who underwent D2 gastrectomy without IPC were enrolled as the control group (group C). All patients had received epidural pain control. The primary endpoints were time to first post-operative flatus and time until oral feeding with a soft diet without discomfort. Secondary endpoints were early complications during hospitalization.
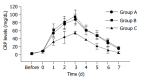
Results: Gender, the type of resection, operating time, blood loss, tumor status and amount of narcotics were comparable in the three groups. However, the group C patients were older than those in groups A and B (67.5+/-17.7 vs 56.8+/-13.2, 57.5+/-11.7 years, P = 0.048). First bowel flatus occurred after 4.35+/-0.93 d in group A, 4.94+/-1.37 d in group B, and 4.71+/-1.22 d in group C (P>0.05). Oral feeding of a soft diet was tolerated 7.21+/-1.92 d after operation in group A, 10.15+/-2.17 d in group B, and 7.53+/-1.35 d in group C (groups A and C vs group B, P<0.05). There was no significant difference in respect to the first flatus among the three groups. However, the time of tolerating oral intake with soft food in groups A and C patients was significantly shorter than that in group B patients. Levels of C-reactive protein (CRP) were significantly lower in group C and there was a more prominent and prolonged response in CRP level in patients undergoing IPC. The incidence of post-operative complications was similar in the three groups except for prolonged post-operative ileus. There was no increased risk of anastomotic leakage in patients receiving Met.
Conclusion: The results suggest that a combination of intravenous Met and epidural pain control may be required to achieve a considerable decrease in time to resumption of oral soft diet in advanced gastric cancer patients who underwent gastrectomy and IPC. Furthermore, the administration of Met did not increase anastomotic leakage. Met has a role in the prevention of prolonged post-operative ileus.
Figures
References
-
- Akoh JA, Macintyre IM. Improving survival in gastric cancer: review of 5-year survival rates in English language publications from 1970. Br J Surg. 1992;79:293–299. - PubMed
-
- Landry J, Tepper JE, Wood WC, Moulton EO, Koerner F, Sullinger J. Patterns of failure following curative resection of gastric carcinoma. Int J Radiat Oncol Biol Phys. 1990;19:1357–1362. - PubMed
-
- Hermans J, Bonenkamp JJ, Boon MC, Bunt AM, Ohyama S, Sasako M, Van de Velde CJ. Adjuvant therapy after curative resection for gastric cancer: meta-analysis of randomized trials. J Clin Oncol. 1993;11:1441–1447. - PubMed
-
- Hallissey MT, Dunn JA, Ward LC, Allum WH. The second British Stomach Cancer Group trial of adjuvant radiotherapy or chemotherapy in resectable gastric cancer: five-year follow-up. Lancet. 1994;343:1309–1312. - PubMed
-
- Hall JJ, Loggie BW, Shen P, Beamer S, Douglas Case L, McQuellon R, Geisinger KR, Levine EA. Cytoreductive surgery with intraperitoneal hyperthermic chemotherapy for advanced gastric cancer. J Gastrointest Surg. 2004;8:454–463. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

