Complicated diverticulitis: is it time to rethink the rules?
- PMID: 16192818
- PMCID: PMC1402355
- DOI: 10.1097/01.sla.0000184843.89836.35
Complicated diverticulitis: is it time to rethink the rules?
Abstract
Introduction: Much of our knowledge and treatment of complicated diverticulitis (CD) are based on outdated literature reporting mortality rates of 10%. Practice parameters recommend elective resection after 2 episodes of diverticulitis to reduce morbidity and mortality. The aim of this study is to update our understanding of the morbidity, mortality, characteristics, and outcomes of CD.
Methods: Three hundred thirty-seven patients hospitalized for CD were retrospectively analyzed. Characteristics and outcomes were determined using chi-squared and Fisher exact tests.
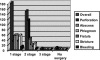
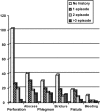
Results: Mean age of patients was 65 years. Seventy percent had one or more comorbidities. A total of 46.6% had a history of at least one prior diverticulitis episode, whereas 53.4% presented with CD as their first episode. Overall mortality rate was 6.5% (86.4% associated with perforation, 9.5% anastomotic leak, 4.5% patient managed nonoperatively). A total of 89.5% of the perforation patients who died had no history of diverticulitis. Steroid use was significantly associated with perforation rates as well as mortality (P< 0.001 and P = 0.002). Comorbidities such as diabetes, collagen-vascular disease, and immune system compromise were also highly associated with death (P = 0.006, P = 0.009, and P = 0.003, respectively). Overall morbidity was 41.4%. Older age, gender, steroids, comorbidities, and perforation were significantly associated with morbidity.
Conclusion: Today, mortality from CD excluding perforation is reduced compared with past data. This, coupled with the fact that the majority of these patients presented with CD as their first episode, calls into question the current practice of elective resection as a stratagem for reducing mortality. Immunocompromised patients may benefit from early resection. New prospective data is needed to redefine target groups for prophylactic resection.
Figures

References
-
- Berry AR, Turner WH, et al. Emergency surgery for complicated diverticular disease: a five year experience. Dis Colon Rectum. 1989;32:849–854. - PubMed
-
- Hackford AW, Schoetz DJ, et al. Surgical management of complicated diverticulitis: the Lahey Clinic experience, 1967 to 1982. Dis Colon Rectum. 1985;28:317–321. - PubMed
-
- Wedell J, Banzhaf G, et al. Surgical management of complicated colonic diverticulitis. Br J Surg. 1997;84:380–383. - PubMed
-
- Lambert ME, Knox RA, et al. Management of the septic complications of diverticular disease. Br J Surg. 1986;73:576–579. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

